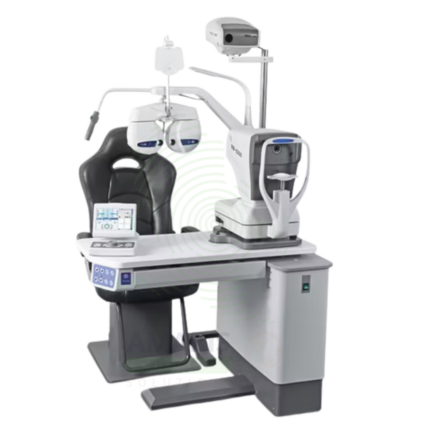
Auto Refractometer
WhatsApp Order
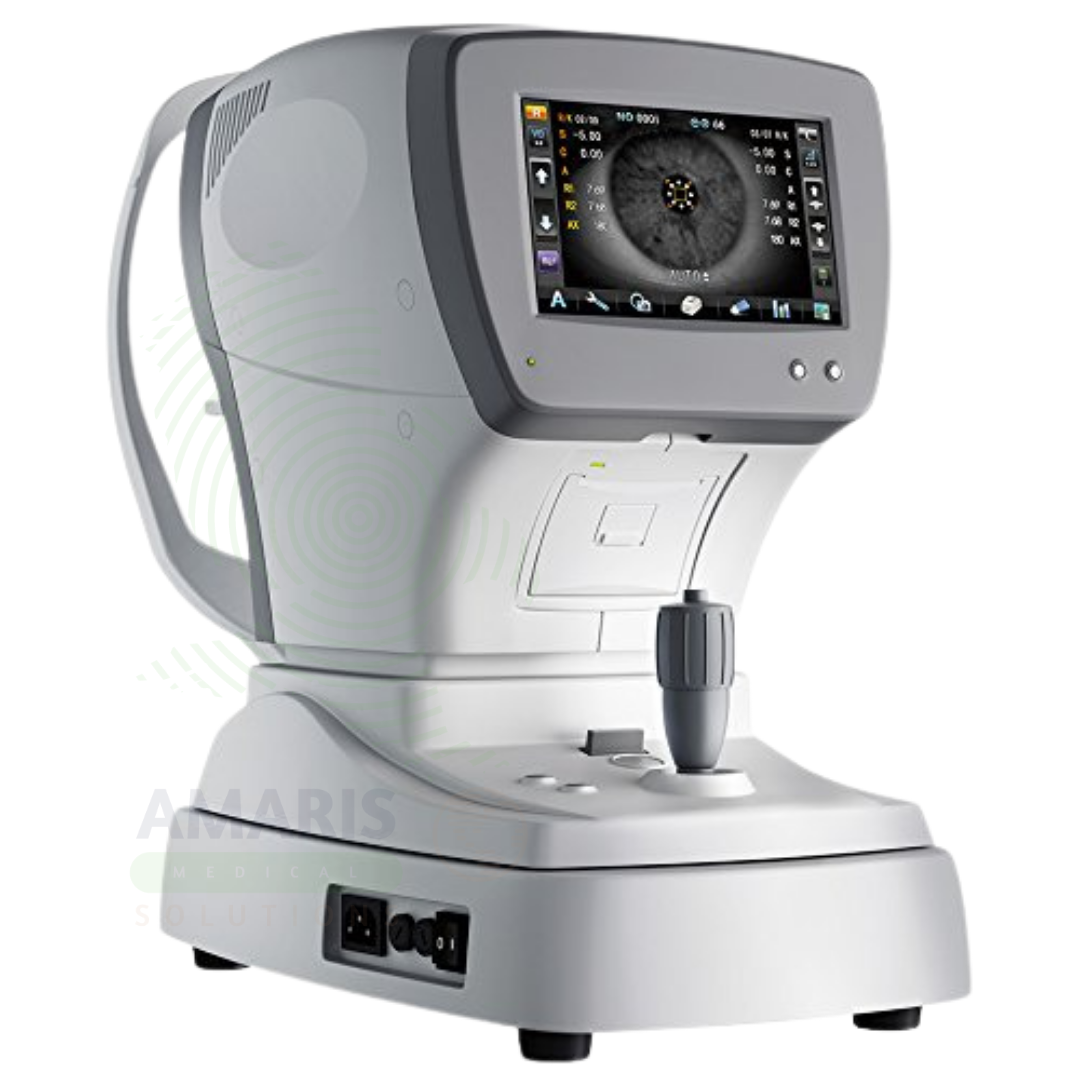
An Auto Refractometer is an automated instrument that objectively measures refractive error, providing accurate readings of sphere, cylinder, and axis for eyeglass and contact lens prescriptions. Using infrared light, it provides non-contact, comfortable measurements that serve as a starting point for subjective refraction. Many models also measure pupil diameter and corneal curvature, offering comprehensive data for contact lens fitting and refractive surgery planning. Essential for optometry and ophthalmology practices.
Description
Auto Refractometer
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Automated Objective Refraction
-
Primary Use: Automatically measures the refractive error of the eye to determine the prescription for glasses or contact lenses. The auto refractometer uses infrared light to measure spherical power, cylindrical power, and axis without requiring subjective patient responses, providing an objective starting point for refraction.
-
How it helps: For the optometrist and ophthalmologist, the auto refractometer provides a quick, objective measurement of refractive error—serving as a valuable starting point for subjective refraction and reducing examination time. For the patient, this means faster, more comfortable examinations with less dependence on subjective responses.
2. Measurement of Spherical, Cylindrical, and Axis Correction
-
Primary Use: Accurately measures sphere (nearsightedness or farsightedness), cylinder (astigmatism), and axis (orientation of astigmatism). The instrument provides precise measurements that guide the final prescription determination.
-
How it helps: For the eye care professional, accurate objective measurements provide a reliable baseline for refraction—reducing the number of trial lenses needed during subjective refraction. For the patient, this means more accurate prescriptions and better visual outcomes.
3. Pupil and Corneal Measurements
-
Primary Use: Many auto refractometers also measure pupil diameter and corneal curvature (keratometry), providing additional data for contact lens fitting, refractive surgery planning, and evaluation of corneal conditions.
-
How it helps: For the optometrist and ophthalmologist, additional measurements provide valuable data for contact lens fitting, refractive surgery evaluation, and assessment of corneal conditions such as keratoconus. For the patient, this means comprehensive measurements in a single device, reducing the need for multiple instruments.
4. Non-Contact Measurement for Patient Comfort
-
Primary Use: Non-contact measurement using infrared light eliminates the need for touching the eye, providing a comfortable experience for patients, particularly those who are anxious about eye examinations.
-
How it helps: For the clinician, non-contact measurement allows rapid, comfortable examinations for all patients, including children and those with anxiety about eye exams. For the patient, this means a comfortable, non-invasive examination experience.
5. Rapid Screening and Pre-Examination Assessment
-
Primary Use: Provides rapid refractive measurements that can be used for screening large populations or as a pre-examination assessment before comprehensive eye examination, allowing practitioners to focus on subjective refinement.
-
How it helps: For the eye care practice, auto refractometry enables efficient patient flow—providing baseline data that streamlines the examination process. For the patient, this means shorter examination times and more efficient use of their time.
SECONDARY & SUPPORTIVE USES
1.Pediatric Refraction: Objective measurement for children who may have difficulty with subjective refraction.
2. Refractive Screening: Rapid screening for refractive errors in school, workplace, or community settings.
3. Pre-Operative Assessment: Baseline measurements for refractive surgery candidates.
4. Contact Lens Fitting: Keratometry measurements for contact lens base curve selection.
5. Glaucoma Screening: Pupil diameter measurement as part of glaucoma evaluation.
6. Research Applications: Refractive measurements for clinical research studies.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: An automated instrument for objective measurement of refractive error.
-
Designation: Auto Refractometer, Automated Refractor, Autorefractor, Objective Refractometer.
-
Key Components:
-
Optical System: Infrared light source and detection system.
-
Fogging System: Relaxes accommodation for accurate measurement.
-
Display: Digital screen showing refractive measurements.
-
Printer: Optional integrated printer for results.
-
Chin Rest: Adjustable chin and forehead rest.
-
Alignment System: Automatic or manual eye alignment.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Measurement Range: -20.00 to +20.00 D (sphere).
-
Cylinder Range: 0 to ±10.00 D.
-
Axis: 0-180 degrees.
-
Pupil Diameter: 2-12 mm.
-
Keratometry: 5-10 mm radius range.
-
Measurement Time: 0.5-2 seconds per eye.
-
Data Output: Printout or electronic transfer.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Benchtop unit with adjustable chin rest.
-
Dimensions: Compact for countertop placement.
-
Controls: Touchscreen or button interface.
-
Portability: Stationary benchtop unit.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Light Safety: Infrared light safe for eyes.
-
Electrical Safety: Compliant with medical electrical equipment standards.
-
Infection Control: Clean chin and forehead rest between patients.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Stored on the countertop in the examination room.
-
Cleaning: Clean chin rest and forehead rest with disinfectant between patients.
-
Calibration: Regular calibration per manufacturer schedule.
-
Maintenance: Professional service as recommended.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Objective measurement of refractive error for eyeglass and contact lens prescriptions.
-
Clinical Role: Essential equipment in optometry and ophthalmology practices.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Patient Positioning: Ensure proper head alignment for accurate measurement.
-
Infection Control: Clean chin rest and forehead rest after each patient.
-
Accommodation Control: Ensure proper fogging to relax accommodation.
-
Children: Use pediatric settings for children; may require additional guidance.
2. FIRST AID MEASURES
-
Eye Irritation: If a patient experiences eye irritation, discontinue use; assess for any injury.
-
Syncope: If patient faints, lower head, elevate legs; monitor vital signs.
3. FIRE FIGHTING MEASURES
-
Flammability: Electrical components may pose fire risk.
-
Extinguishing Media: For electrical fire, use CO₂ or dry chemical extinguisher.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties