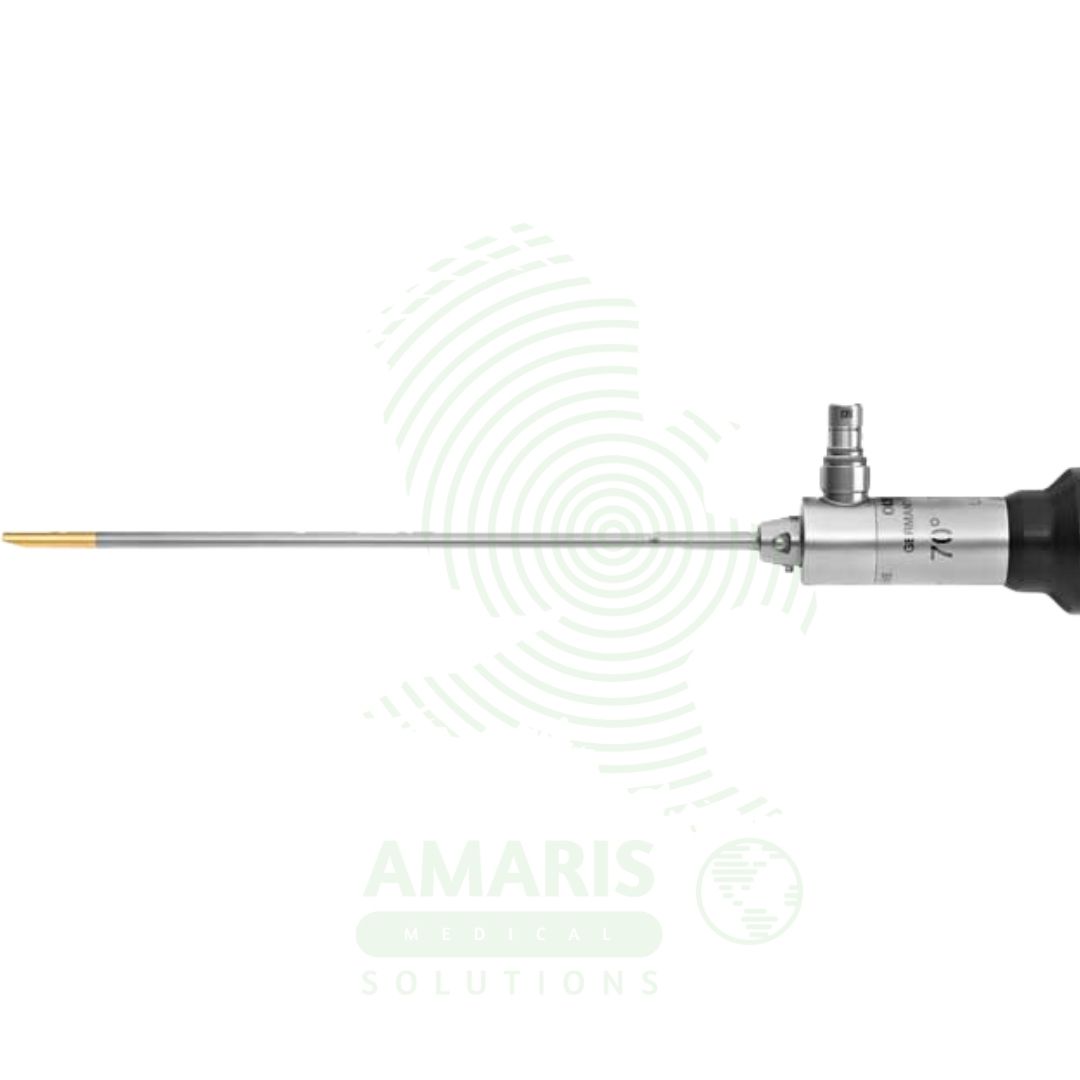
Orthopedic Arthroscope
WhatsApp Order
An Orthopedic Arthroscope is a rigid, rod-lens telescope used for the visualization and surgical treatment of joint interiors. As the cornerstone of minimally invasive joint surgery, it provides a bright, magnified view of structures like cartilage, menisci, and ligaments through tiny incisions. Available in key diameters (2.7mm, 4.0mm) and viewing angles (0°, 30°, 70°), its optical quality is paramount for surgical precision. Mandatory pre-sterilization leak testing and careful autoclaving are required to maintain sterility and integrity. Proper handling is essential to prevent costly damage to the optics and to ensure patient safety during diagnostic and therapeutic arthroscopic procedures.
Description
Orthopedic Arthroscope
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Diagnostic Arthroscopy
-
Primary Use: Provides direct, magnified visualization of the interior of a joint (synovium, articular cartilage, menisci, ligaments, tendons) to diagnose the source of pain, swelling, locking, or instability when non-invasive imaging is inconclusive.
-
How it helps: For the orthopedic surgeon, the arthroscope transforms joint diagnosis from indirect imaging to direct visualization—revealing the exact condition of cartilage, the precise location of a meniscal tear, the true state of a ligament, or the source of unexplained synovitis. For the patient suffering from chronic knee pain, shoulder instability, or hip impingement, diagnostic arthroscopy often provides the definitive answer that MRI and X-ray could not, guiding treatment with certainty.
2. Therapeutic Joint Surgery (Arthroscopic Surgery)
-
Primary Use: Enables minimally invasive surgical interventions within the joint, performed through small “keyhole” portals, across multiple joints including knee, shoulder, hip, ankle, elbow, and wrist.
-
How it helps: For the orthopedic surgeon, the arthroscope is both eyes and instrument—allowing them to repair torn menisci, reconstruct cruciate ligaments, debride damaged cartilage, and stabilize shoulders through incisions measured in millimeters rather than inches. For the athlete sidelined by an ACL tear, the worker unable to lift due to rotator cuff injury, or the aging adult limited by meniscal pathology, arthroscopic surgery means their joint can be repaired through minimally invasive techniques, with less pain, faster rehabilitation, and earlier return to the activities they love.
3. Knee Arthroscopy
-
Primary Use: Performs meniscectomy, meniscal repair, ACL/PCL reconstruction, cartilage debridement, microfracture, loose body removal, and synovectomy through small portals.
-
How it helps: For the knee surgeon, the arthroscope provides access to all compartments of this complex joint—visualizing the torn meniscus catching and locking, the absent ACL causing instability, or the cartilage defect causing pain. For the patient with a locked knee from a bucket-handle meniscal tear, or the athlete whose knee gives way from ACL insufficiency, arthroscopic repair offers the chance to restore function and return to activity without the morbidity of open arthrotomy.
4. Shoulder Arthroscopy
-
Primary Use: Performs rotator cuff repair, subacromial decompression, labral repair, biceps tenodesis, and stabilization for recurrent dislocation.
-
How it helps: For the shoulder surgeon, the arthroscope navigates the complex anatomy of the glenohumeral joint and subacromial space—repairing torn rotator cuff tendons, debriding impinging bone spurs, and stabilizing recurrently dislocating shoulders. For the patient unable to lift their arm due to rotator cuff tear, or the young athlete with recurrent shoulder instability, arthroscopic repair offers the hope of restored function and stability without the large incisions and extensive soft tissue dissection of open surgery.
SECONDARY & SUPPORTIVE USES
1. Biopsy Guidance: For the orthopedic surgeon evaluating unexplained synovitis or suspected intra-articular pathology, the arthroscope allows precise, targeted biopsy of synovial tissue for histopathological diagnosis. For the patient with pigmented villonodular synovitis, inflammatory arthritis, or suspected infection, arthroscopic biopsy provides diagnostic tissue with minimal morbidity.
2. Irrigation and Debridement: In septic arthritis, the arthroscope enables thorough joint lavage to remove purulent material and debride fibrinous exudate, potentially saving the joint from rapid destruction. For the patient with an infected joint, arthroscopic washout offers a minimally invasive way to clear infection while preserving joint function.
3. Assessment and Treatment of Fractures: Arthroscopic assistance aids in the assessment and reduction of intra-articular fractures, ensuring that joint surfaces are anatomically aligned. For the patient with a tibial plateau, radial head, or other intra-articular fracture, arthroscopic visualization helps the surgeon restore the smooth joint surface essential for long-term function and prevention of post-traumatic arthritis.
4. Post-Operative Assessment and Lysis of Adhesions: Second-look arthroscopy allows assessment of healing after meniscal repair or cartilage procedures, and arthroscopic release of adhesions can treat arthrofibrosis causing joint stiffness. For the patient with persistent stiffness after surgery or injury, arthroscopic lysis of adhesions can restore motion without the trauma of open release.
5. Joint Stabilization Procedures: For patients with multidirectional instability or recurrent dislocation, arthroscopic visualization enables capsular plication or thermal capsulorrhaphy to tighten lax tissues. For the individual whose shoulder dislocates with simple daily activities, arthroscopic stabilization offers the chance for secure, stable function without the morbidity of open procedures.
6. Tendon and Cyst Evaluation: Arthroscopic techniques extend beyond joints to procedures like endoscopic carpal tunnel release and ganglion cyst excision. For the patient with carpal tunnel syndrome, endoscopic release offers faster recovery and less scar tenderness than open release, while ganglion excision through small portals minimizes cosmetic and functional impact.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A rigid, rod-lens optical telescope specifically designed for insertion into joints through a small cannula.
-
Designation: Defined by its application (arthroscopy) and its optical specifications.
-
Core Specifications:
-
Diameter: Common sizes are 2.7mm (small joints: wrist, ankle, pediatric), 4.0mm (standard for knee, shoulder), and 5.0mm (larger joints or for specific optics).
-
Length: Varies by joint; typically 10-18cm.
-
Angle of View: The direction the lens looks relative to the long axis of the scope. Critical for accessing different areas of a joint.
-
0° (Forward Viewing): Provides a straightforward, panoramic view. Excellent for orientation and general visualization.
-
30° (Angled): The most commonly used. The lens is angled at 30°, allowing the surgeon to look "around corners" by rotating the scope, greatly increasing the field of view without moving the portal.
-
70° (Wide-Angle): Used for specialized visualization, such as looking into the posterior knee compartment or the acetabulum in hip arthroscopy.
-
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Optical System: Utilizes a Hopkins rod-lens system for superior light transmission, image clarity, brightness, and wide field of view compared to traditional lens systems.
-
Field of View: The angular extent of the observable scene (e.g., 60°-90°).
-
Depth of Field: The range of distances that remain in sharp focus, allowing clear visualization from the joint capsule to the far side of the joint.
-
Light Guide Post: Connects to a high-intensity fiber-optic light cable from a xenon or LED light source to illuminate the dark joint cavity.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Made of high-grade, medical stainless steel for durability, rigidity, and to withstand repeated sterilization.
-
Integration: Attaches to a medical video camera head for display on a monitor (video arthroscopy). Older systems may have a direct eyepiece.
-
Trocar/Cannula Compatibility: Designed to pass through a specific diameter arthroscopic cannula or sheath, which maintains the portal and allows for inflow/outflow.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Classified as a Class I medical device.
-
Biocompatibility & Sterility: Must be fully sterilizable (via autoclave) and made of biocompatible materials for internal use within a sterile surgical field.
-
Optical Integrity: Lenses must be free of cracks, chips, clouding, or delamination. Even minor defects can scatter light and severely distort the image, posing a surgical risk.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a protective container or dedicated rack within a sterilization tray to prevent damage to the delicate tip and lenses. Avoid contact with other metal instruments.
-
Cleaning & Sterilization (CRITICAL):
-
Immediate Post-Use: Clean the external surface meticulously to remove biological debris.
-
Leak Testing: Must be performed before every sterilization cycle to check for breaches in the sealed outer sheath. Fluid ingress can cause cross-infection and destroy the optics.
-
Sterilization: Autoclave (steam sterilization) is the standard. Follow manufacturer's precise instructions for time, temperature, and drying cycles to prevent damage.
-
-
Handling: Always handle with extreme care. Never drop. Hold by the robust body, never by the eyepiece, camera adapter, or the distal tip. Use protective tips when not in use.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: The essential visual instrument for all arthroscopic (minimally invasive joint) surgeries across orthopedic subspecialties (knee, shoulder, hip, sports medicine).
-
Clinical Role: The "eyes" of the arthroscopic surgeon, enabling precise diagnosis and complex intra-articular surgery through portals less than 1cm in size, reducing tissue trauma, pain, and recovery time compared to open surgery.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Thermal Injury: The metal shaft of the scope can conduct heat from the light cable or from proximity to electrosurgical/radiofrequency probes, potentially causing cartilage or capsular burns. Awareness of scope position is key.
-
Cartilage Scuffing (Iatrogenic Damage): The sharp, metallic tip can scratch articular cartilage if inserted or moved carelessly. Always insert the scope through a cannula and move it gently within the joint.
-
Scope Breakage: Although rare, the scope can break under extreme torque or if struck. Do not use excessive force when navigating tight joints.
-
Image Artifacts: Fogging, bleeding, or debris on the lens can obscure vision. Use scope warmers, adequate irrigation pressure, and lens cleaners to maintain a clear view. A blurry image is a safety hazard.
-
Portal Placement: Incorrect portal placement can lead to poor visualization, instrument clash, and increased risk of neurovascular injury. Proper preoperative planning and anatomical knowledge are essential.
2. FIRST AID MEASURES
-
Broken Scope Tip in Joint: If the distal tip breaks, do not remove the cannula. Keep the fragment in view on the monitor. Use a grasper through a separate portal to retrieve all pieces meticulously. Confirm retrieval with fluoroscopy if necessary.
-
Significant Cartilage Damage: If iatrogenic cartilage scuffing occurs, debride the unstable edges and document the incident. The long-term impact is assessed post-operatively.
-
Loss of Visualization During Critical Step: If the image is lost (e.g., due to fogging or massive bleeding), the surgeon should announce "hold," keep instruments stationary, and have the assistant troubleshoot (clean lens, adjust inflow) before proceeding.
3. FIRE FIGHTING MEASURES
-
Flammability: The scope itself is non-combustible metal and glass. Attached light cables may have combustible components.
-
Extinguishing Media: Use appropriate extinguishing media (CO2 for electrical) for any fire source in the OR.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties