Spinal Needles
WhatsApp Order
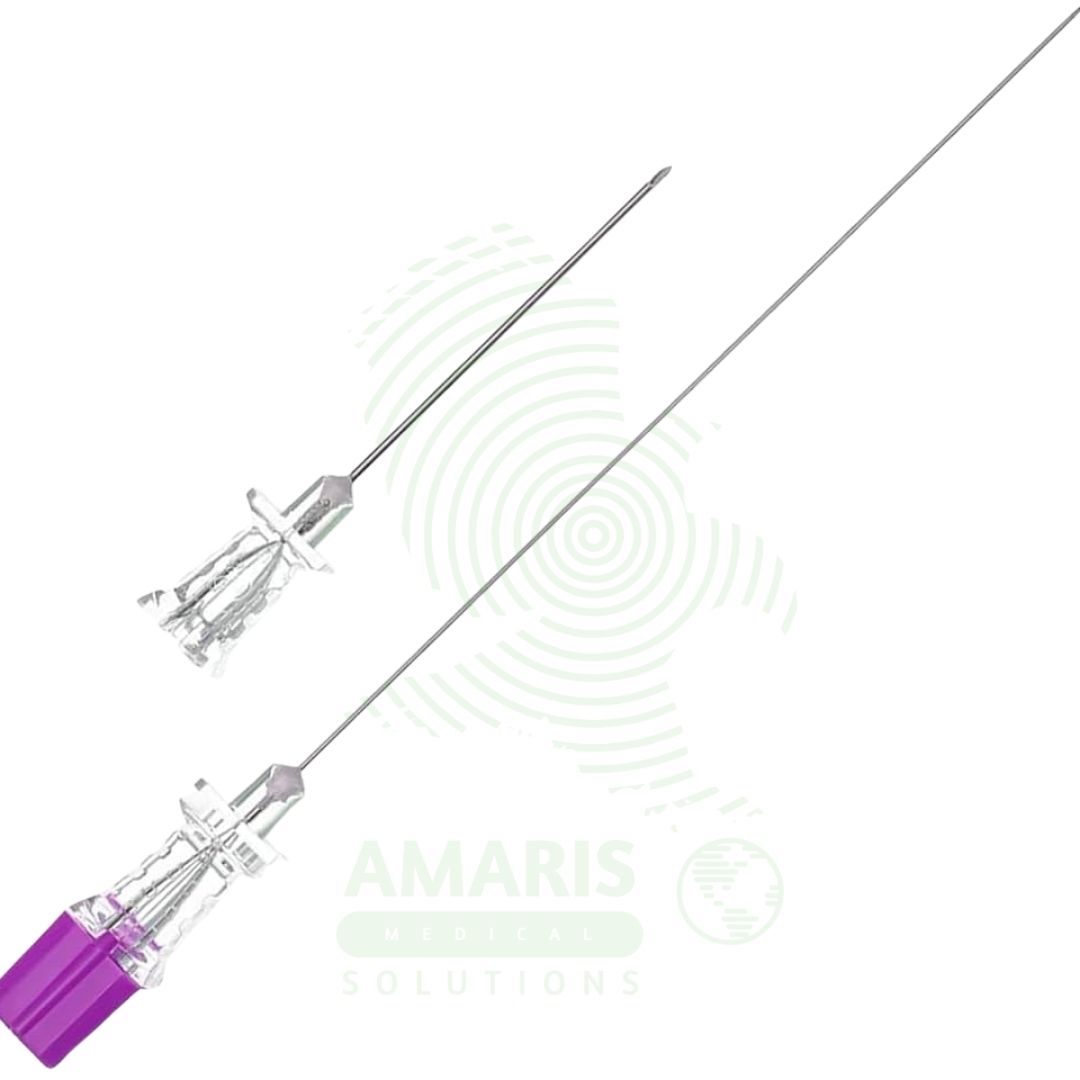
A Spinal Needles is a specialized, hollow-bore needle used to access the cerebrospinal fluid in the subarachnoid space for anesthesia, diagnosis, or therapy. Its design is critical: modern pencil-point tips (e.g., Whitacre) minimize the risk of post-dural puncture headache compared to older cutting bevels. Needle gauge (22G-27G) balances procedural ease with complication risk. Its use demands absolute aseptic technique, precise anatomical knowledge, and careful management of potentially life-threatening complications such as high spinal anesthesia or neurological injury. It is a fundamental, high-risk/high-reward tool in anesthesiology, neurology, and emergency medicine.
Description
Spinal Needles
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Spinal Anesthesia (Subarachnoid Block)
-
Primary Use: Injects local anesthetic directly into the cerebrospinal fluid within the subarachnoid space to achieve rapid, dense sensory, motor, and autonomic blockade for surgical procedures below the diaphragm, most commonly for cesarean sections, lower limb orthopedic surgery, and urological and gynecological procedures.
-
How it helps: For the anesthesiologist, the spinal needle provides access to the cerebrospinal fluid—a conduit to the central nervous system where a small dose of local anesthetic can produce complete surgical anesthesia from the waist down. For the patient undergoing cesarean section, hip replacement, or prostate surgery, spinal anesthesia means they can remain awake and comfortable during their procedure, avoiding the risks of general anesthesia and experiencing excellent post-operative pain control.
2. Diagnostic Lumbar Puncture
-
Primary Use: The definitive diagnostic procedure to collect cerebrospinal fluid for laboratory analysis to diagnose conditions such as meningitis, encephalitis, subarachnoid hemorrhage, multiple sclerosis, and leptomeningeal carcinomatosis, and to measure intracranial pressure.
-
How it helps: For the neurologist and emergency physician, the spinal needle is the tool that unlocks the diagnostic secrets held in cerebrospinal fluid—revealing the bacteria causing meningitis, the blood from subarachnoid hemorrhage, or the inflammatory markers of multiple sclerosis. For the patient with severe headache, fever, altered mental status, or suspected neurological disease, the lumbar puncture often provides the definitive diagnosis that guides life-saving treatment or provides answers that end diagnostic uncertainty.
3. Therapeutic Lumbar Puncture
-
Primary Use: Used to relieve elevated intracranial pressure or to administer intrathecal chemotherapy for hematologic malignancies or leptomeningeal disease.
-
How it helps: For the neurosurgeon and oncologist, the spinal needle provides access for both removing pressure-causing fluid and delivering chemotherapy directly to the central nervous system—treating conditions that systemic medications cannot reach. For the patient with idiopathic intracranial hypertension causing debilitating headaches and vision threat, removing CSF provides immediate symptom relief. For the child with leukemia, intrathecal chemotherapy delivered through a spinal needle protects the central nervous system from malignant cells, dramatically improving survival.
4. Myelography
-
Primary Use: Injects radiopaque contrast medium into the subarachnoid space prior to X-ray, CT, or fluoroscopic imaging to visualize the spinal cord, nerve roots, and meninges for diagnosing spinal stenosis, herniated discs, or tumors.
-
How it helps: For the radiologist and spine surgeon, myelography transforms the spinal canal from a radiographically invisible space into a clearly outlined structure—revealing where the cord or nerves are compressed by herniated discs, narrowed canals, or tumors. For the patient with radicular pain, spinal stenosis, or suspected cord compression, this imaging guides surgical planning and ensures that interventions target the correct level and pathology.
SECONDARY & SUPPORTIVE USES
1. Combined Spinal-Epidural (CSE) Anesthesia: For the anesthesiologist managing labor analgesia or major surgery, the CSE technique uses a spinal needle passed through an epidural needle to deliver rapid-onset spinal anesthesia while leaving an epidural catheter for prolonged coverage. For the woman in labor, this means rapid pain relief when she needs it most, with the ability to extend analgesia throughout delivery and beyond.
2. Intrathecal Drug Administration: For the pain specialist and neurologist, spinal needles enable the administration of medications directly into the CSF—antibiotics for CNS infections, baclofen for severe spasticity, or opioids for chronic pain via implanted pumps. For the patient with cerebral palsy and debilitating spasticity, or with chronic pain unresponsive to oral medications, intrathecal drug delivery can provide relief that transforms quality of life.
3. Spinal Drain Placement: For the neurosurgeon managing CSF leaks or elevated pressure post-neurosurgery, spinal needles facilitate the placement of drains for continuous CSF drainage. For the patient with a postoperative CSF leak or refractory intracranial hypertension, this drainage can prevent complications, promote healing, and avoid additional surgery.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A long, thin, hollow-bore needle specifically designed for puncturing the dura mater to access the subarachnoid space.
-
Designation: Defined by its tip design (most critical feature) and its gauge (diameter).
-
Core Tip Designs:
-
Quincke (Cutting Bevel): A sharp, pencil-point tip with a beveled cutting edge. Traditional design, higher incidence of Post-Dural Puncture Headache (PDPH). The bevel orientation (parallel to dural fibers) is important.
-
Whitacre, Sprotte, Gertie Marx (Pencil-Point/Non-Cutting): A solid, rounded pencil-point tip with the side opening (eyehole) proximal to the tip. The tip separates rather than cuts dural fibers, significantly reducing the risk of PDPH. This is the modern standard for most procedures, especially in obstetrics.
-
Atraucan (Blunt Tip): Similar to pencil-point, designed to minimize trauma.
-
-
Key Specifications:
-
Gauge (G): Diameter. Common sizes are 22G, 25G, and 27G. Smaller gauge (higher number) = lower risk of PDPH but slower CSF flow.
-
Length: Typically 3.5 inches (90mm) for most adults.
-
Stylet: A solid, removable wire that fits inside the needle to prevent coring of skin and tissue during insertion, ensuring a clean puncture. Its fit must be perfect.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
CSF Flow Rate: Determined by needle gauge and length (Poiseuille's Law). A 22G needle provides rapid, unmistakable CSF return. A 27G needle requires patience and often hanging a drop of fluid at the hub to confirm.
-
Flexibility: Very fine-gauge needles (27G+) are flexible, requiring an introducer needle (a shorter, larger-gauge needle) to provide rigidity for penetrating the tough interspinous ligament and ligamentum flavum.
-
Huber Point: Many spinal needles feature a Huber point (a closed, non-coring tip) to prevent tissue plugging.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Packaging: Sterile, single-use, with a stylet pre-inserted. Often color-coded by gauge.
-
Hub Design: Clear hub to visualize CSF ("flash").
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Classified as a Class II or III medical device (high risk due to entry into CNS).
-
Sterility: Must be supplied sterile. Aseptic technique is non-negotiable.
-
Biocompatibility: Must be non-toxic and non-pyrogenic.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry place. Protect from crushing or bending.
-
Handling: Use strict aseptic technique. Do not touch the shaft. Inspect for damage before use.
-
Disposal: After use, it is a sharps hazard and must be disposed of immediately in an approved, puncture-proof sharps container.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: The essential instrument for anesthesiologists, neurologists, and emergency physicians to access the cerebrospinal fluid for anesthesia, diagnosis, and therapy.
-
Clinical Role: Enables one of the most fundamental and high-stakes procedures in medicine, where precision and minimization of complications are paramount.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Absolute Asepsis: The procedure must be performed under sterile conditions with full barrier precautions (mask, cap, sterile gloves, gown, large sterile drape). Skin preparation with chlorhexidine-alcohol is standard.
-
Correct Patient Positioning: Optimal flexion of the lumbar spine (lateral decubitus or sitting) is critical to open the interlaminar spaces. Anatomical landmarks must be carefully identified.
-
Gauge and Tip Selection: Use the smallest gauge, pencil-point needle appropriate for the procedure to minimize PDPH risk, especially in young, female, and obstetric populations.
-
Stylet Re-insertion: The stylet must be re-inserted before withdrawing the needle to prevent seeding of epithelial cells into the CSF track, which can cause epidermoid tumors.
-
Aspiration and Injection: Gently aspirate to confirm free CSF flow before injecting any medication. Inject slowly. Never inject if blood is aspirated (indicating vascular puncture).
-
Monitoring: Continuous monitoring of vital signs (especially for hypotension/bradycardia from spinal anesthesia) and neurological status is mandatory.
-
Contraindications: Absolute contraindications include patient refusal, infection at the puncture site, coagulopathy, and increased intracranial pressure from a mass lesion.
2. FIRST AID MEASURES
-
High/Total Spinal Anesthesia: If local anesthetic spreads too high, causing respiratory distress, apnea, or severe bradycardia/hypotension: Call for help, secure airway (intubate), ventilate, and provide cardiovascular support (fluids, vasopressors like phenylephrine/ephedrine, atropine).
-
Post-Dural Puncture Headache (PDPH): Manage with conservative measures (fluids, caffeine, analgesics). For severe or persistent headache, an epidural blood patch is the definitive treatment.
-
Neurological Injury/Spinal Hematoma: Suspected if new, progressive motor/sensory deficits or bowel/bladder dysfunction occur post-procedure. This is a neurosurgical emergency. Immediate spinal imaging (MRI) and consultation are required.
-
Infection (Meningitis): If signs of CNS infection develop (fever, neck stiffness, photophobia), perform diagnostic workup and initiate broad-spectrum antibiotics immediately.
3. FIRE FIGHTING MEASURES
-
Flammability: Packaging is combustible.
-
Extinguishing Media: Use appropriate media for the surrounding fire.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties