Chest Bottle
WhatsApp Order
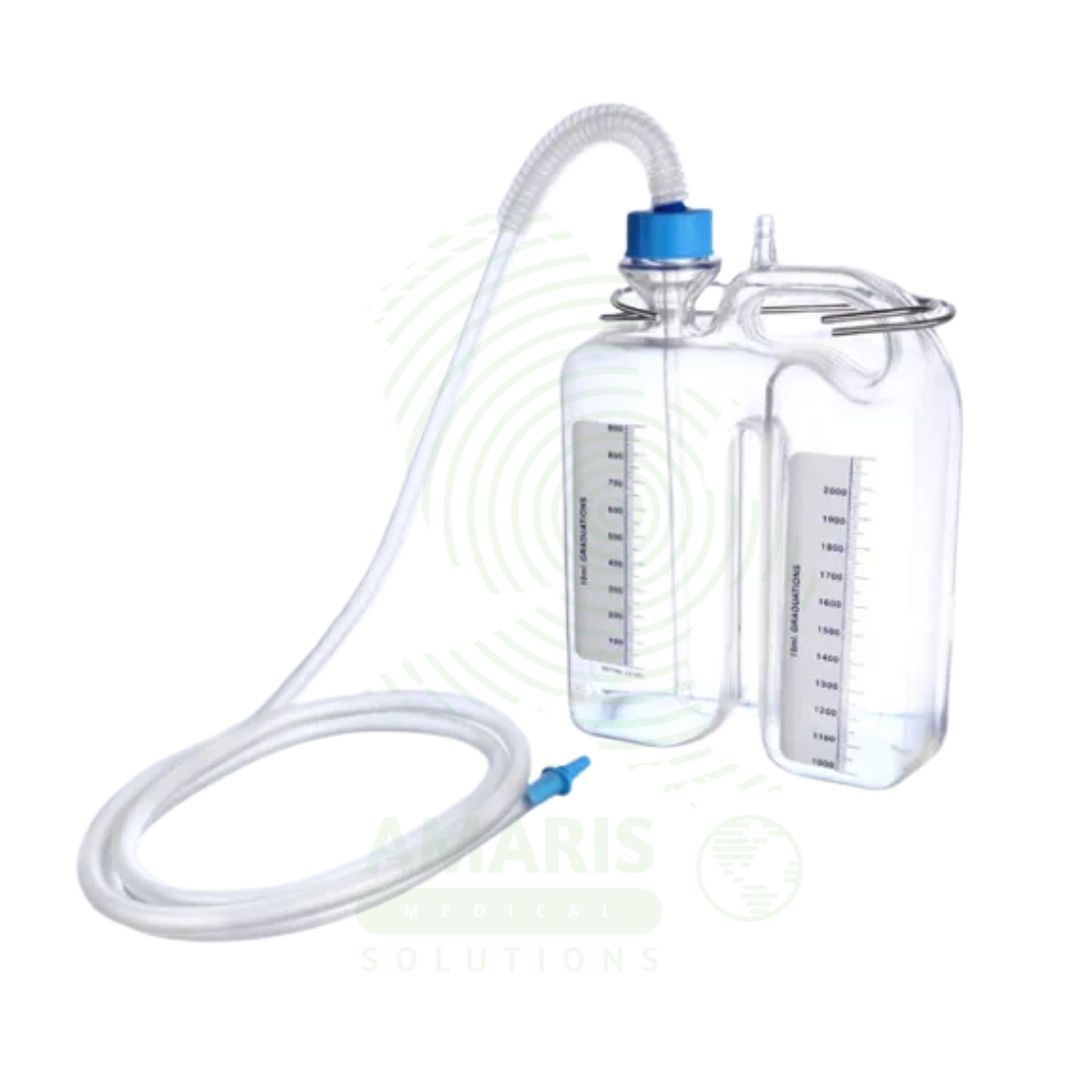
A Chest Bottle (Underwater Seal Drainage System) is a three-chamber disposable device used to drain air and fluid from the pleural space via a chest tube. Its critical component is a water seal chamber that acts as a one-way valve, preventing air from re-entering the chest while allowing drainage. It is used to treat pneumothorax, hemothorax, and pleural effusions, and is mandatory post-thoracic surgery. The system must always be kept upright and below the patient’s chest level. It provides essential clinical information through tidaling in the water seal (indicating tube patency and lung expansion) and bubbling (indicating an air leak), making it both a therapeutic and diagnostic tool.
Description
Chest Bottle
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Underwater Seal Drainage of the Pleural Cavity
-
Primary Use: Provides a one-way valve for air and fluid (blood, effusion, chyle, empyema) draining from a patient’s pleural space via a chest tube, preventing atmospheric air from being sucked back into the chest during inspiration.
-
How it helps: For the surgeon, pulmonologist, or intensive care nurse, the underwater seal is a simple yet elegant physiological solution—it lets unwanted contents leave the chest but absolutely nothing return. For the patient with a collapsed lung or fluid around their lung, this mechanism ensures that as they breathe in, they draw air into their lungs, not back into the pleural space, allowing the lung to gradually re-expand and heal.
2. Treatment of Pneumothorax
-
Primary Use: Evacuates air from the pleural space, allowing a collapsed lung to re-expand, with bubbling in the water seal chamber indicating an ongoing air leak.
-
How it helps: For the clinician managing a pneumothorax, the chest bottle transforms an invisible physiological problem into a visible one—bubbles tell the story of air leaking from the lung. For the patient who arrived gasping with a collapsed lung, watching bubbles travel through the tube provides tangible evidence that the trapped air is escaping and their lung has room to breathe again.
3. Treatment of Hemothorax, Pleural Effusion, and Empyema
-
Primary Use: Allows for the controlled drainage of blood, serous fluid, or pus from the pleural cavity, monitoring the volume and rate of output.
-
How it helps: For the trauma surgeon or medical team, the graduated collection chamber provides continuous feedback—how much blood is this patient losing? Is the effusion draining? Is the infection clearing? For the patient, each milliliter drained is fluid that was compressing their lung, making every breath a little easier as the chest bottle slowly restores space for their lung to expand.
4. Post-Operative Thoracic Drainage
-
Primary Use: Standard following thoracic surgeries (lobectomy, pneumonectomy, cardiac surgery) to drain residual air and fluid, monitor for bleeding, and ensure lung re-expansion.
-
How it helps: For the cardiothoracic surgical team, the chest bottle is their window into the chest after they’ve closed it—watching for post-op bleeding, air leaks from suture lines, or proper lung re-expansion. For the patient waking from heart or lung surgery, this silent companion by the bedside is working continuously to clear the surgical site, prevent complications, and help them breathe deeply as they begin their recovery.
SECONDARY & SUPPORTIVE USES
1. Measurement of Output: For the nursing and medical team, the calibrated collection chamber allows precise measurement of fluid volume and character—distinguishing between expected post-op drainage, concerning hemorrhage, or signs of infection. For the patient, accurate output monitoring ensures that complications are caught early, before they become emergencies.
2. Assessment of Air Leak: For the respiratory therapist or surgeon, the water seal chamber provides a visual window into lung healing—continuous bubbling suggests a significant air leak from lung parenchyma, while intermittent bubbling with cough is normal. For the patient with a lung injury or recent surgery, the gradual decrease and cessation of bubbling over days signals that their lung is sealing and healing as it should.
3. Application of Controlled Suction: For the clinician managing complex drainage, the suction control chamber allows precise negative pressure application (typically -10 to -20 cm H₂O) to enhance drainage and lung expansion. For the patient with a persistent pneumothorax or large effusion, gentle suction actively encourages the lung to re-expand and hold against the chest wall, speeding recovery and reducing time with a chest tube in place.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A disposable, rigid plastic, three-chamber collection system used in conjunction with a chest tube.
-
Common Names: Often called an "Underwater Seal Drainage System," "Pleurovac," or "Chest Drainage Unit."
-
Core Chambers & Function:
-
Collection Chamber: The first chamber. Receives fluid and air directly from the patient via the chest tube. It is calibrated to measure output (in mL).
-
Water Seal Chamber: The second and most critical chamber. Contains sterile water (typically filled to the 2cm mark). The tube from the collection chamber dips 2cm below the water surface, creating a one-way seal. This chamber shows tidaling (fluctuation with respiration) and bubbling (air leak).
-
Suction Control Chamber: The third chamber. Used when suction is applied. Filled with water to a level (e.g., -20 cm) that determines the maximum negative pressure applied to the pleural space. Bubbling in this chamber indicates suction is being applied.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Calibration: Clear, accurate mL markings on the collection chamber for measuring output.
-
Water Seal Depth: Standard 2 cm H2O. This is the minimum pressure needed to overcome the seal and allow air to escape from the pleural space.
-
Suction Control Setting: Adjustable by adding or removing water (e.g., -10, -15, -20 cm H2O). The suction source must be set high enough to cause gentle, continuous bubbling in this chamber.
-
High-Volume Capacity: Collection chambers can typically hold 2000-2500 mL of fluid before requiring emptying/replacement.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Connections: Standardized tubing connectors: a patient port (from chest tube), a suction port (to wall vacuum), and an atmospheric vent.
-
Stability: Designed with a wide base and often a hanger to be positioned below the patient's chest level (on the floor or bed rail) at all times to maintain the water seal.
-
Transparency: Made of clear plastic for continuous visual assessment of all chambers.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Classified as a Class II medical device.
-
Sterility: The system is supplied sterile, and the water added to the seal and suction chambers must be sterile.
-
One-Way Valve Integrity: The underwater seal is a passive, fail-safe mechanism. The system must remain upright and intact to maintain this seal.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry area in its sealed package.
-
Setup: Must be set up and filled with sterile water according to strict aseptic technique before connection to the patient's chest tube.
-
Handling During Use: The unit must always be kept upright and below the level of the patient's chest. Tilting or raising it above the chest can cause fluid to flow back into the pleural space.
-
Disposal: Once disconnected from the patient, the entire unit is disposed of as biohazardous/clinical waste due to contamination with bodily fluids.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: The standard of care for managing chest tubes in thoracic surgery, pulmonology, emergency medicine, and critical care.
-
Clinical Role: A critical monitoring and therapeutic device that provides both treatment (drainage) and continuous diagnostic information (air leak, output volume) for pleural space pathologies.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Position is Paramount: The bottle must always be kept below chest level. Elevating it will cause siphoning of fluid back into the pleural cavity, risking infection or tamponade.
-
Maintain Water Seal: Never empty the water seal chamber while the system is connected to the patient. The water level must be checked and maintained at the 2cm mark.
-
Tube Patency: Ensure the chest tube and all connecting tubing are not kinked, compressed, or clogged. Monitor for tidaling in the water seal chamber; absence of tidaling may indicate tube obstruction, lung re-expansion, or system malfunction.
-
Clamping Chest Tubes: Clamp chest tubes only under specific, directed circumstances (e.g., to quickly assess for a persistent air leak, or to change the drainage system). Never clamp for transport or without a clear clinical reason, as it can rapidly cause a tension pneumothorax.
-
Sudden Cessation of Bubbling/Tidaling: This may indicate lung re-expansion (desired) or tube obstruction (dangerous). Assess the patient clinically (breath sounds, oxygenation) and the system immediately.
2. FIRST AID MEASURES
-
Accidental Disconnection at Patient Port: Immediately clamp the chest tube close to the patient's body (if a clamp is at hand), ask the patient to exhale and hold it if possible, and reconnect the tubing using aseptic technique. The exposed end of the chest tube can be temporarily submerged in a bottle of sterile water to create an emergency seal.
-
Bottle Tip-Over/Breakage: If the system is compromised, clamp the chest tube temporarily. Replace the entire drainage system as quickly as possible using a new, pre-set-up unit.
-
Tension Pneumothorax Suspected (Patient in Distress): This is a clinical emergency. If a tension pneumothorax is suspected due to system malfunction or occlusion, immediately decompress the chest with a needle thoracostomy if necessary, following emergency protocols. Do not wait.
3. FIRE FIGHTING MEASURES
-
Flammability: Plastic components are combustible.
-
Extinguishing Media: Use water, CO2, or foam as appropriate for the surrounding fire.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties