Endobronchial Tubes
WhatsApp Order
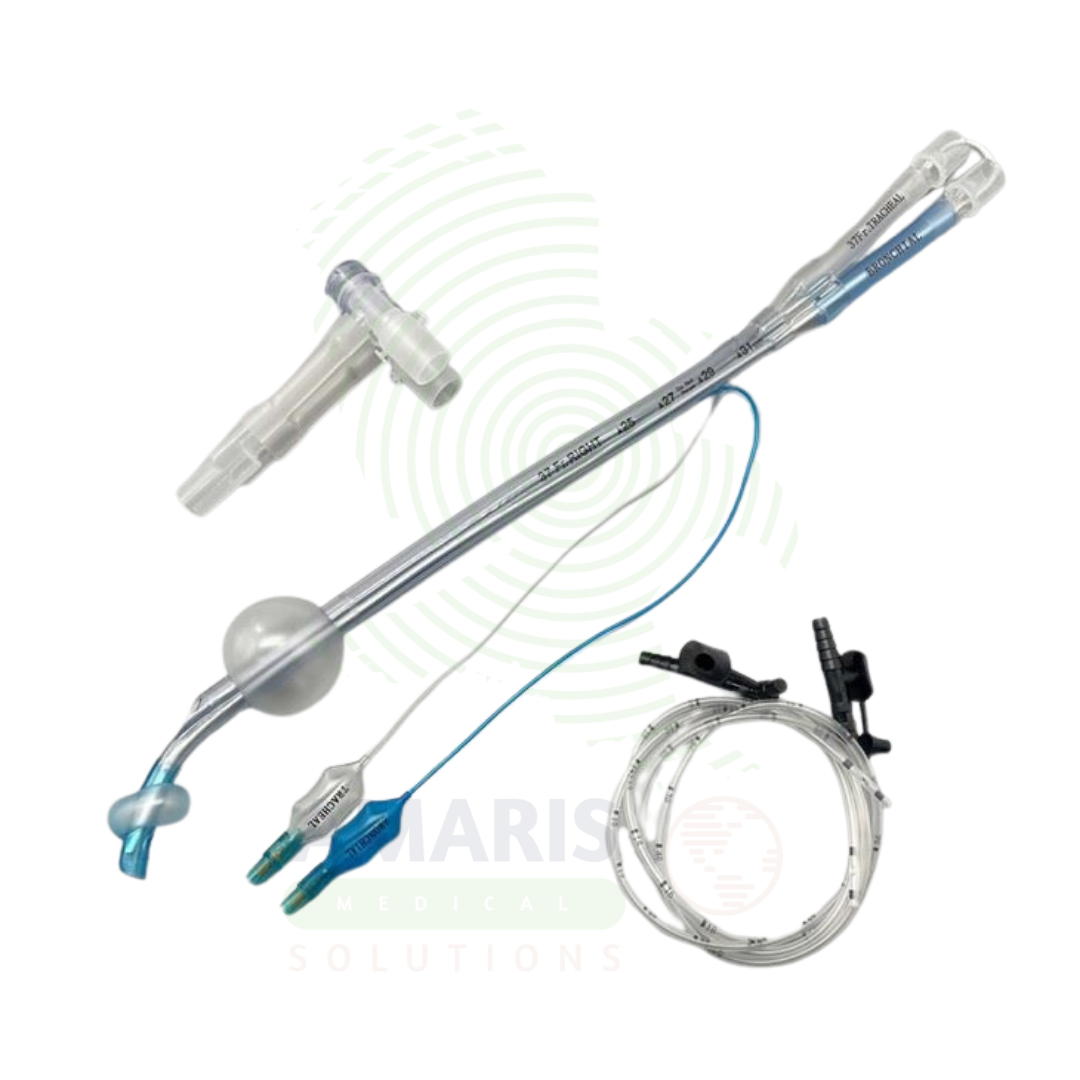
Endobronchial Tubes are specialized double-lumen endotracheal tubes designed for selective lung ventilation and isolation during thoracic surgery, management of massive hemoptysis, and bronchopleural fistulas. The dual-lumen design allows independent ventilation of each lung, enabling surgical access, infection control, and airway protection. Essential for thoracic surgery, anesthesiology, and critical care, they provide safe, effective single-lung ventilation with proper placement confirmed by fiberoptic bronchoscopy.
Description
Endobronchial Tubes
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Selective Lung Ventilation for Thoracic Surgery
-
Primary Use: Provides selective ventilation of one lung while allowing the other lung to be collapsed during thoracic surgical procedures including lobectomy, pneumonectomy, esophagectomy, and video-assisted thoracoscopic surgery. The double-lumen tube design allows independent ventilation of the left and right lungs.
-
How it helps: For the thoracic surgeon and anesthesiologist, endobronchial tubes enable optimal surgical access by selectively deflating the lung on the operative side while maintaining ventilation to the contralateral lung—providing a clear surgical field and protecting the healthy lung from contamination. For the patient undergoing thoracic surgery, this technology allows for minimally invasive approaches, reduces operative time, and minimizes the risk of complications associated with single-lung ventilation.
2. Isolation of the Lung for Infection Control
-
Primary Use: Isolates a lung affected by infection, hemorrhage, or massive abscess to prevent spillage of infectious material or blood into the healthy lung during surgical or therapeutic procedures.
-
How it helps: For the thoracic surgeon and anesthesiologist, endobronchial tubes provide a critical barrier that contains infectious or hemorrhagic material within the diseased lung—protecting the healthy lung from contamination and preventing life-threatening aspiration. For the patient with severe pulmonary infection or massive hemoptysis, this isolation can be life-saving, allowing for definitive treatment while preserving respiratory function.
3. Management of Bronchopleural Fistula
-
Primary Use: Used to manage bronchopleural fistulas by selectively isolating the affected bronchus, preventing air leak into the pleural space and maintaining adequate ventilation.
-
How it helps: For the critical care team and thoracic surgeon, endobronchial tubes provide a means of managing this challenging complication—sealing off the fistulous communication and allowing the pleural space to heal. For the patient with a bronchopleural fistula, proper tube placement can prevent respiratory compromise and facilitate healing without additional surgical intervention.
4. Facilitation of Bronchoscopic Procedures
-
Primary Use: Provides a conduit for passage of fiberoptic bronchoscopes for diagnostic and therapeutic procedures, including lavage, biopsy, and laser therapy, while maintaining ventilation.
-
How it helps: For the interventional pulmonologist, endobronchial tubes allow simultaneous access for bronchoscopic instruments and maintenance of ventilation—enabling complex airway interventions without interrupting gas exchange. For the patient undergoing bronchoscopic procedures, this means safer, more efficient interventions with continuous respiratory support.
5. Management of Massive Hemoptysis
-
Primary Use: Used in the emergency management of massive hemoptysis to isolate the bleeding lung and prevent aspiration of blood into the contralateral airway.
-
How it helps: For the emergency physician and critical care team, endobronchial tube placement provides immediate airway protection in life-threatening hemoptysis—containing the bleeding source and maintaining a patent airway for ventilation. For the patient with massive hemoptysis, this intervention can be life-saving, preventing asphyxiation and allowing time for definitive treatment.
SECONDARY & SUPPORTIVE USES
1. Difficult Airway Management: Used in complex airway scenarios where conventional endotracheal intubation is challenging or where selective ventilation is required for airway control.
2. Tracheobronchial Trauma: Provides airway stabilization and selective ventilation in patients with traumatic injury to the tracheobronchial tree.
3. Lung Transplantation: Used during lung transplantation procedures to selectively ventilate the transplanted lung while the native lung is managed.
4. Pulmonary Lavage: Facilitates whole-lung lavage in patients with pulmonary alveolar proteinosis by allowing sequential lavage of one lung while the other is ventilated.
5. Thoracic Trauma: Used in the acute management of thoracic trauma where lung isolation is required to prevent contamination or manage air leaks.
6. Pediatric Applications: Smaller endobronchial tubes are available for pediatric thoracic surgery and airway management in children.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A specialized double-lumen endotracheal tube designed for selective lung ventilation and isolation.
-
Designation: Endobronchial Tube, Double-Lumen Tube, DLT, Bronchial Catheter, Carlens Tube, Robertshaw Tube.
-
Key Components:
-
Dual Lumens: Separate channels for ventilation of each lung (tracheal lumen and bronchial lumen).
-
Bronchial Cuff: Inflatable cuff that seals the bronchus of the ventilated lung.
-
Tracheal Cuff: Inflatable cuff that seals the trachea, preventing air leak and aspiration.
-
Bronchial Tip: Extended tip designed to enter the main bronchus (left or right specific).
-
Pilot Balloons: Color-coded balloons for monitoring cuff inflation.
-
Radiopaque Markers: Positioned to confirm correct placement under fluoroscopy or X-ray.
-
Connectors: Standard 15 mm connectors for ventilator circuits.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Sizes: 26 Fr to 41 Fr for adults; pediatric sizes available.
-
Lumen Diameter: Varies by size; sufficient for passage of fiberoptic bronchoscope.
-
Cuff Types: High-volume, low-pressure cuffs to minimize tracheal and bronchial injury.
-
Material: Medical-grade polyvinyl chloride (PVC) or silicone.
-
Radiopacity: Embedded markers for radiographic confirmation.
-
Direction: Left-sided or right-sided configuration based on intended placement.
-
Sterility: Ethylene oxide or gamma irradiation sterilized.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Flexible but kink-resistant tubing; smooth surface for atraumatic insertion.
-
Color Coding: Blue for tracheal cuff, white or clear for bronchial cuff.
-
Length: 28-40 cm depending on size.
-
Markings: Depth markings at 1 cm intervals for accurate placement.
-
Packaging: Sterile, single-use; individually packaged.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Biocompatibility: Materials safe for airway contact.
-
Cuff Safety: High-volume, low-pressure cuffs reduce risk of mucosal ischemia.
-
Latex-Free: Manufactured without natural rubber latex.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry location at room temperature.
-
Sterility Maintenance: Do not use it if the package is opened, damaged, or wet.
-
Expiration: Check expiration date before use; do not use after expiration.
-
Single-Use Only: Intended for single patient use only; do not resterilize or reuse.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Selective lung ventilation and isolation for thoracic surgery, massive hemoptysis, and bronchopleural fistula management.
-
Clinical Role: Essential equipment in thoracic surgery, anesthesiology, and critical care settings.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Confirm Placement: Verify correct position with fiberoptic bronchoscopy after intubation.
-
Cuff Inflation: Inflate cuffs to minimal occluding volume; monitor cuff pressures.
-
Tube Security: Secure tube after confirming placement to prevent dislodgement.
-
Position Monitoring: Monitor for signs of tube migration, obstruction, or malposition.
-
Suctioning: Suction both lumens as needed to maintain patency.
-
Deflation Prior to Removal: Deflate cuffs completely before extubation.
2. FIRST AID MEASURES
-
Tube Displacement: If tube is displaced, manually ventilate patient; remove tube; reintubate as needed.
-
Cuff Rupture: If cuff ruptures, consider tube replacement if the seal cannot be maintained.
-
Obstruction: If lumen is obstructed, attempt to suction; consider tube replacement if patency cannot be restored.
3. FIRE FIGHTING MEASURES
-
Flammability: Plastic components are combustible; an oxygen-enriched environment increases fire risk.
-
Extinguishing Media: For electrical fire, use CO₂ or dry chemical extinguisher.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties