Inhaler Spacer with Child Mask
WhatsApp Order
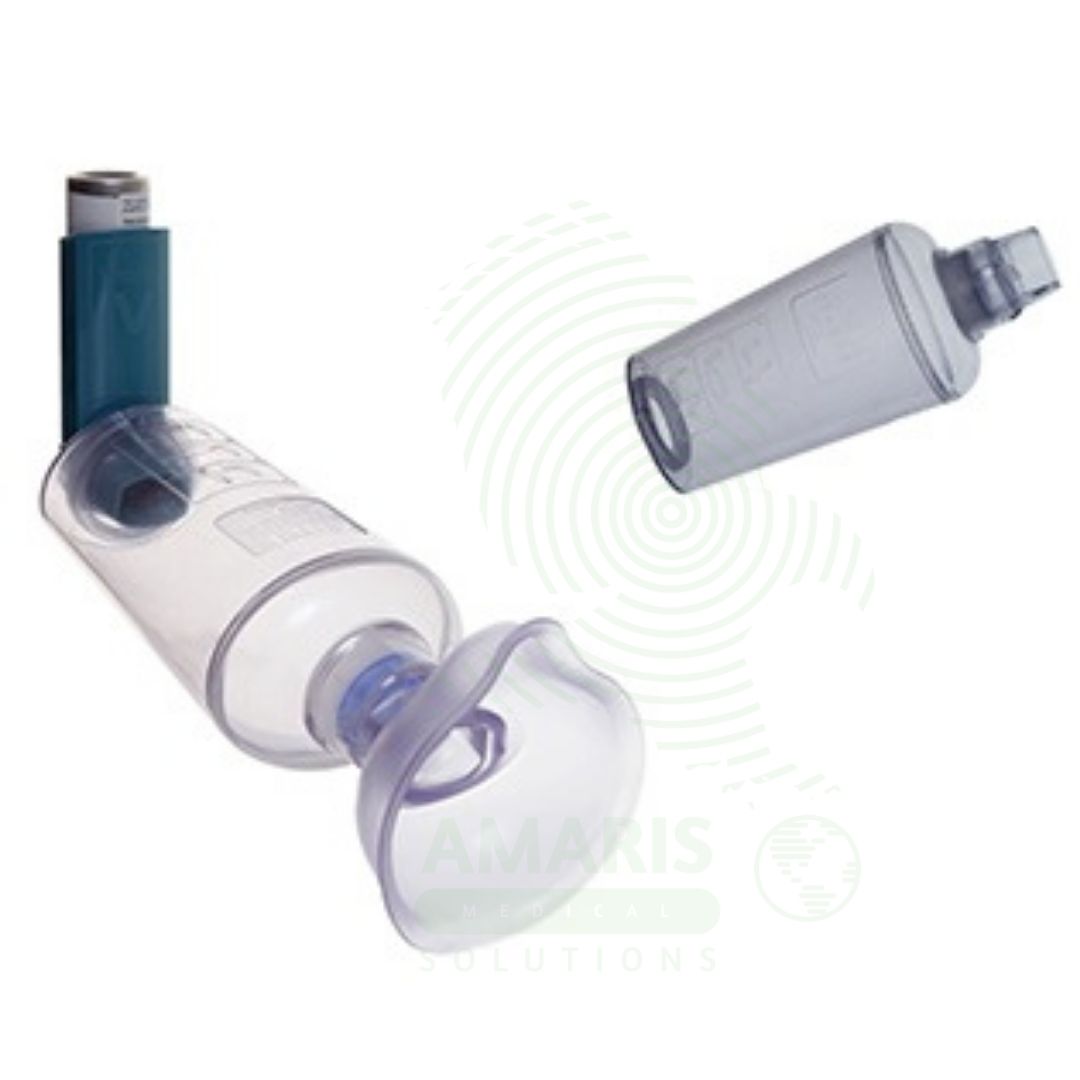
An Inhaler Spacer with Child Mask is a valved holding chamber designed to optimize aerosol medication delivery from metered-dose inhalers to infants and young children. The spacer captures the medication spray, allowing the child to inhale over multiple breaths, while the soft mask creates a seal over the nose and mouth. This improves pulmonary drug deposition, reduces oropharyngeal side effects, and eliminates the need for complex breath coordination. Essential for pediatric asthma management, the spacer enables effective inhaler use in children as young as infancy, supporting home management of reactive airway disease.
Description
Inhaler Spacer with Child Mask
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Optimization of Aerosol Medication Delivery in Children
-
Primary Use: Attaches to a metered-dose inhaler to hold the aerosolized medication in a holding chamber, allowing the child to inhale the medication over multiple breaths rather than requiring coordination of actuation with inhalation. The spacer improves drug delivery to the lungs and reduces oropharyngeal deposition.
-
How it helps: For the pediatrician and respiratory therapist, the spacer with a child mask transforms a difficult-to-use inhaler into an effective delivery system—eliminating the need for a young child to coordinate breathing with medication actuation and ensuring that the medication reaches the lungs rather than being deposited in the mouth and throat. For the child with asthma, the spacer means they can receive their medication effectively even if they cannot follow complex instructions, turning a stressful experience into a simple, passive treatment.
2. Improvement of Pulmonary Drug Deposition
-
Primary Use: Slows the velocity of aerosol particles and allows the propellant to evaporate, reducing the size of particles that reach the airways. This increases the fraction of medication deposited in the lungs and reduces the amount deposited in the oropharynx.
-
How it helps: For the clinician managing a child with asthma or reactive airway disease, the spacer ensures that more of the medication reaches the small airways where it is needed—improving bronchodilation, reducing inflammation, and achieving better clinical outcomes with lower doses. For the child, better drug delivery means more effective symptom relief and potentially fewer medication side effects from swallowed or deposited drug.
3. Reduction of Oropharyngeal Deposition and Systemic Absorption
-
Primary Use: By capturing larger aerosol particles in the chamber, the spacer prevents deposition of medication in the mouth and throat, reducing local side effects such as oral candidiasis (thrush) and dysphonia, as well as systemic absorption from swallowed medication.
-
How it helps: For the pediatric nurse and family managing a child on inhaled corticosteroids, the spacer is essential for preventing thrush and other local side effects that can discourage treatment adherence. For the child, reduced oral deposition means fewer side effects and a more comfortable treatment experience, making daily medication more tolerable.
4. Facilitation of Inhaler Use in Young Children
-
Primary Use: The child mask creates a seal over the nose and mouth, allowing infants and young children who cannot use a mouthpiece to receive aerosolized medication. The mask eliminates the need for the child to coordinate inhalation with actuation, making inhaler therapy possible in children as young as infancy.
-
How it helps: For the parents of a young child with asthma or wheezing, the spacer with a child mask means they can administer life-saving bronchodilators and anti-inflammatory medications to their child even during a respiratory crisis when the child is too distressed to coordinate breathing. For the infant or toddler, the soft, comfortable mask allows them to receive their medication while seated in a parent’s lap, turning a potentially frightening experience into a calm, manageable routine.
5. Enhancement of Treatment Adherence in Pediatric Asthma
-
Primary Use: Simplifies the medication administration process, reducing the complexity and skill required to use a metered-dose inhaler effectively. This improves adherence to prescribed therapy and reduces the need for nebulizer treatments in many children.
-
How it helps: For the pediatric asthma educator and primary care provider, prescribing a spacer with a child mask increases the likelihood that families will correctly administer prescribed medications—simplifying the process, reducing errors, and improving long-term asthma control. For the family managing a child’s asthma, the spacer means less time spent on treatments, fewer struggles during medication administration, and better control of their child’s symptoms.
SECONDARY & SUPPORTIVE USES
1. Use in Acute Asthma Exacerbations: The spacer with mask allows for rapid administration of bronchodilators during acute wheezing episodes in children, providing relief without the need for a nebulizer machine.
2. Home-Based Asthma Management: Enables families to manage childhood asthma at home with the same device used in clinical settings, supporting early intervention during symptom flares.
3. Administration of Other Aerosolized Medications: Can be used to deliver other metered-dose inhaler medications including inhaled corticosteroids, combination products, and rescue bronchodilators.
4. Use in Special Needs Populations: The mask design makes the spacer suitable for children and adults with developmental disabilities or conditions that make mouthpiece use difficult.
5. Travel and Portable Use: Compact and lightweight, the spacer with mask provides a portable solution for families managing asthma during travel, school, and daily activities.
6. Emergency Department and Urgent Care: Used in acute care settings for rapid administration of bronchodilators to children presenting with wheezing, providing an alternative to nebulizer treatments.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A valved holding chamber with a face mask designed for use with metered-dose inhalers in children who cannot use a mouthpiece.
-
Designation: Inhaler Spacer, Valved Holding Chamber, Aerochamber, Pediatric Spacer with Mask, MDI Spacer.
-
Key Components:
-
Spacer Chamber: Plastic holding chamber that captures and holds aerosol medication from the metered-dose inhaler.
-
Child Mask: Soft, flexible silicone or latex-free mask that seals over the child's nose and mouth.
-
Inhaler Port: Connection point on the back of the spacer where the metered-dose inhaler is inserted.
-
One-Way Valve: Located at the mouthpiece end or within the chamber; allows medication to flow toward the patient but prevents exhaled air from entering the chamber.
-
Retainer Ring: Holds the metered-dose inhaler securely in place during actuation.
-
Tidal Breathing Indicator (select models): A whistle or flow indicator that signals if the child is breathing too quickly or too slowly.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Particle Retention: Traps large, non-respirable particles while allowing respirable particles to reach the patient.
-
Dead Space Volume: Minimal dead space to ensure maximum drug delivery.
-
Valve Function: Low-resistance valve that opens with minimal inspiratory flow, suitable for infants and young children.
-
Mask Seal: Soft, flexible mask that conforms to facial contours to maintain seal during treatment.
-
Material: Anti-static plastic to reduce electrostatic charge that can retain medication particles.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Chamber Volume: Typically 100-200 mL for pediatric spacers.
-
Mask Sizes: Available in small, medium, and large to accommodate infants through school-age children.
-
Mask Material: Soft silicone or latex-free plastic; hypoallergenic.
-
Connector: Universal fitting compatible with most metered-dose inhalers.
-
Cleaning: Dishwasher safe or washable with mild soap and water.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Latex-Free: Many models manufactured without natural rubber latex to reduce allergic reaction risk.
-
Electrostatic Protection: Anti-static materials prevent medication adherence to chamber walls.
-
Material Safety: All patient-contact materials biocompatible and non-toxic.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry place; protect from extreme temperatures.
-
Cleaning: Wash with mild dish soap and warm water; rinse thoroughly; air dry before use. Do not use alcohol-based cleaners. Clean weekly.
-
Mask Care: Inspect mask for damage or wear; replace if cracks or tears develop.
-
Replacement: Spacers should be replaced periodically per manufacturer recommendations; masks replaced if damaged.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Delivery of metered-dose inhaler medications to infants, toddlers, and young children with asthma and reactive airway disease.
-
Clinical Role: Standard of care for pediatric inhaler administration; reduces need for nebulizer treatments.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Mask Seal: Ensure mask forms a good seal over nose and mouth during treatment; leaks reduce medication delivery.
-
Valve Function: Verify valve opens with patient inhalation; check for stuck or damaged valves before use.
-
Cleaning: Do not use alcohol-based cleaners that may damage plastic; do not use harsh detergents.
-
Electrostatic Charge: New spacers may require pre-treatment or washing to reduce static charge that can trap medication.
-
Medication Deposition: Invert spacer after inhalation; do not leave medication standing in the chamber.
-
Inhaler Priming: Prime metered-dose inhaler before first use or if not used recently per manufacturer instructions.
2. FIRST AID MEASURES
-
Medication Spray in Eyes: If medication sprays into eyes, rinse thoroughly with water; seek medical attention if irritation persists.
-
Mask Discomfort: If mask causes facial irritation, check for damage; clean mask thoroughly; consider alternative mask size or material.
-
Inhalation Difficulty: If a child struggles to inhale through spacer, check valve function and mask seal; ensure the child is calm and breathing normally.
3. FIRE FIGHTING MEASURES
-
Flammability: Plastic components are combustible; MDI canisters may contain flammable propellant.
-
Extinguishing Media: Use water, foam, or CO₂ as appropriate for surrounding materials.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties