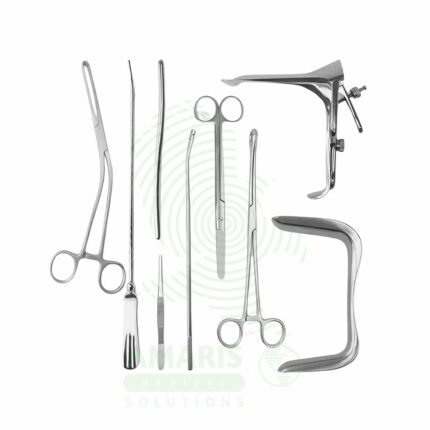
Resectoscope
WhatsApp Order
A Resectoscope is a specialized endoscopic instrument used for transurethral resection of the prostate, bladder tumors, and endometrium. Combining a telescope, working element, and resecting loop, it enables precise cutting and coagulation of tissue under direct visualization. Essential in urology for benign prostatic hyperplasia and bladder cancer treatment, and in gynecology for endometrial resection, it provides minimally invasive treatment with rapid recovery and preservation of organ function.
Description
Resectoscope
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Transurethral Resection of the Prostate
-
Primary Use: Provides a combined visualization and resection system for transurethral resection of the prostate, the classic surgical treatment for benign prostatic hyperplasia. The resectoscope allows the surgeon to visualize the prostate and resect obstructive tissue using a wire loop with electrosurgical current.
-
How it helps: For the urologist, the resectoscope provides the means to remove obstructive prostate tissue through the urethra—eliminating the need for open surgery, reducing hospital stay, and allowing rapid return to normal activities. For the aging man whose quality of life is diminished by frequent urination, weak stream, and nighttime awakening, TURP offers durable relief and return to normal voiding function.
2. Transurethral Resection of Bladder Tumor
-
Primary Use: Used for transurethral resection of bladder tumors, the standard procedure for the diagnosis, staging, and therapeutic resection of bladder tumors. The resectoscope enables complete visualization of the bladder and precise resection of tumor tissue.
-
How it helps: For the urologic oncologist, the resectoscope allows simultaneous visualization and resection of bladder tumors—cutting away abnormal tissue while cauterizing the base, providing tissue for pathological staging, and treating the disease in a single procedure. For the patient with bladder cancer, TURBT offers both diagnosis and initial treatment through a minimally invasive approach, with rapid recovery and preservation of bladder function.
3. Transurethral Incision of the Prostate
-
Primary Use: Used for transurethral incision of the prostate, a less invasive alternative to TURP for patients with smaller prostates. The resectoscope creates incisions in the prostate to relieve obstruction while preserving more tissue.
-
How it helps: For the urologist managing patients with moderate prostatic obstruction, TUIP provides effective relief with fewer side effects and shorter recovery than traditional TURP. For the patient, this means less risk of retrograde ejaculation and faster return to normal activities.
4. Endometrial Resection and Ablation
-
Primary Use: Used in gynecology for transcervical resection of the endometrium and submucous fibroids. The resectoscope provides visualization and resection capability for treatment of abnormal uterine bleeding and fibroids.
-
How it helps: For the gynecologist, the resectoscope offers a minimally invasive alternative to hysterectomy for treatment of menorrhagia and submucous fibroids—preserving the uterus and allowing rapid recovery. For the patient with heavy menstrual bleeding, endometrial resection provides relief while avoiding major surgery and preserving fertility when appropriate.
5. Urethral Stricture Incision
-
Primary Use: Used for direct visualization and incision of urethral strictures using a cold knife or laser through the resectoscope. This minimally invasive approach treats urethral narrowing without open surgery.
-
How it helps: For the urologist, resectoscopic stricture incision offers a minimally invasive treatment for urethral strictures—restoring urinary flow without the morbidity of open urethroplasty. For the patient, this means rapid recovery and preservation of erectile function.
SECONDARY & SUPPORTIVE USES
1. Bladder Neck Incision: Incision of bladder neck contracture following prostate surgery.
2. Ureteral Meatotomy: Incision of stenotic ureteral meatus.
3. Prostatic Stent Placement: Placement of temporary or permanent stents under direct visualization.
4. Laser Prostate Surgery: Resectoscope compatible with laser fibers for holmium laser enucleation of the prostate.
5. Bipolar Resection: Modern resectoscopes with bipolar technology for safer resection with normal saline irrigation.
6. Office-Based Procedures: Smaller resectoscopes for office-based diagnostic and therapeutic procedures.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A specialized endoscopic instrument combining a telescope, working element, and resecting loop for transurethral resection procedures.
-
Designation: Resectoscope, TURP Set, TURBT Set, Transurethral Resectoscope.
-
Key Components:
-
Telescope: Rod lens system with angled optics (typically 12°, 30°, or 70°).
-
Working Element: Mechanism for advancing and retracting the resecting loop.
-
Resecting Loop: Wire loop for cutting and coagulating tissue.
-
Sheath: Outer tube with inflow/outflow channels for irrigation.
-
Light Source: Fiberoptic or LED illumination.
-
Electrosurgical Generator: Provides cutting and coagulation current.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Sheath Diameter: 24-28 French for standard resectoscopes.
-
Telescope Diameter: 4 mm.
-
Viewing Angle: 12°, 30°, or 70° optics.
-
Resecting Loop: Monopolar or bipolar; various loop sizes.
-
Irrigation: Continuous flow for clear visualization.
-
Electrosurgery: Cutting and coagulation modes.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Precision-machined stainless steel.
-
Ergonomics: Designed for single-handed operation.
-
Sterilization: Steam autoclave compatible.
-
Portability: Fixed in operating room setup.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Biocompatibility: Materials safe for intraurethral and intravesical use.
-
Electrical Safety: Compliant for use with electrosurgical generators.
-
Fluid Management: Systems to prevent fluid overload (TUR syndrome).
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in protective cases; protect lenses from damage.
-
Cleaning: Thorough cleaning after each use; ultrasonic cleaning recommended.
-
Sterilization: Steam autoclave per manufacturer instructions.
-
Inspection: Inspect for lens damage, loop integrity, and insulation defects.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Transurethral resection of prostate, bladder tumors, and endometrium.
-
Clinical Role: Essential in urology and gynecology for minimally invasive resection procedures.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Fluid Management: Monitor fluid deficit to prevent TUR syndrome (hyponatremia, fluid overload).
-
Electrosurgical Safety: Use appropriate grounding pad; monitor for stray current.
-
Loop Integrity: Inspect resecting loop for damage before use.
-
Irrigation: Maintain continuous flow for clear visualization and cooling.
-
Anticoagulation: Assess bleeding risk before procedure.
2. FIRST AID MEASURES
-
TUR Syndrome: If signs of fluid overload (nausea, confusion, bradycardia), stop procedure; administer diuretics; monitor electrolytes.
-
Capsular Perforation: If perforation occurs, stop procedure; assess for extravasation; convert to open if needed.
-
Bleeding: If significant bleeding occurs, cauterize; may require transfusion or conversion.
3. FIRE FIGHTING MEASURES
-
Flammability: Metal components are non-flammable; plastic parts may burn.
-
Extinguishing Media: Use water, foam, or CO₂ as appropriate for surrounding materials.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties