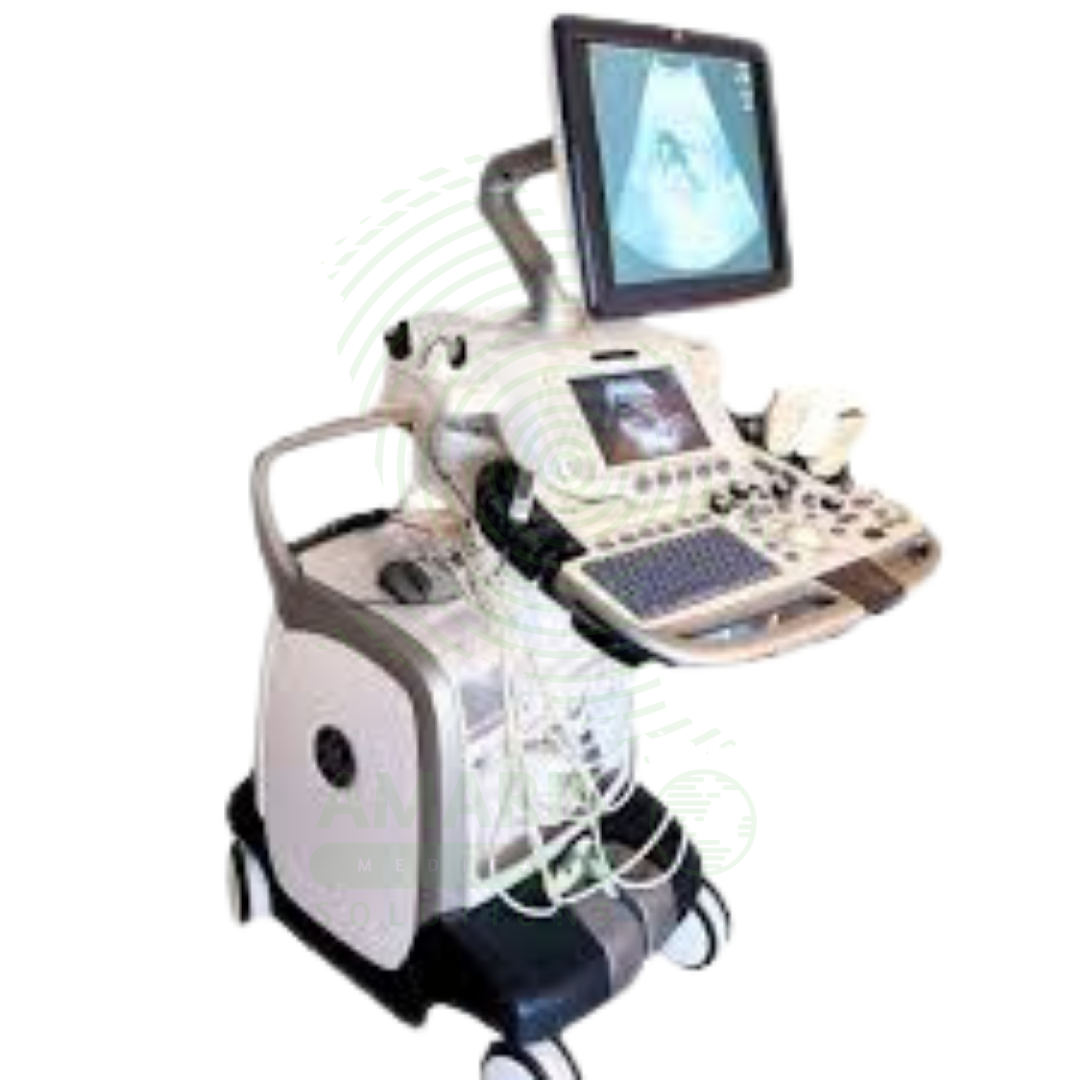
Ultrasound Machine
WhatsApp Order
The Ultrasound Machine is a diagnostic imaging system that uses high-frequency sound waves to produce real-time, dynamic images of internal body structures, including soft tissues, organs, blood vessels, and developing fetuses. It provides non-invasive, radiation-free visualization using multiple transducer probes for abdominal, cardiac, obstetric, gynecological, vascular, and musculoskeletal examinations. With core features like B-mode grayscale imaging, M-mode for motion assessment, and comprehensive Doppler capabilities (Color, Power, Spectral), it offers essential diagnostic functionality for evaluating anatomy, physiology, and blood flow. Its portability, digital image storage, and user-friendly interface make it a practical tool for hospitals, clinics, emergency departments, and point-of-care settings across virtually all medical specialties, requiring proper operator training and adherence to probe disinfection protocols for safe and effective use.
Description
Ultrasound Machine
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Real-Time Anatomical and Physiological Imaging
-
Primary Use: Generates dynamic, real-time images of soft tissue structures and organs using high-frequency sound waves, providing a versatile, non-invasive, and radiation-free tool for visualizing muscles, tendons, internal organs, blood vessels, and developing fetuses.
-
How it helps: For the radiologist, sonographer, and clinician, the ultrasound machine transforms sound waves into living images of the human body—revealing organs in motion, blood flowing through vessels, and developing life in the womb, all without exposing the patient to radiation. For the patient, an ultrasound examination means their internal anatomy can be visualized safely, painlessly, and in real time, providing immediate answers and often the first glimpse of an unborn child.
2. Obstetrics and Gynecology
-
Primary Use: Essential for monitoring fetal development, evaluating the uterus and ovaries for conditions like fibroids and cysts, and guiding gynecological procedures.
-
How it helps: For the obstetrician and maternal-fetal medicine specialist, ultrasound provides a window into the womb—dating pregnancies, assessing fetal anatomy for anomalies, monitoring growth, and evaluating placental position, all critical for ensuring healthy outcomes. For the expectant parent, ultrasound offers the first images of their baby, providing reassurance of normal development and creating a profound early connection. For the gynecology patient, ultrasound reveals the cause of pelvic pain or abnormal bleeding, guiding diagnosis and treatment.
3. Abdominal and Pelvic Imaging
-
Primary Use: Used to assess organs such as the liver, gallbladder, kidneys, pancreas, spleen, bladder, and prostate for conditions like gallstones, cysts, tumors, ascites, and hydronephrosis.
-
How it helps: For the gastroenterologist, urologist, and primary care physician, abdominal ultrasound provides a rapid, non-invasive assessment of solid organs—revealing gallstones causing pain, hydronephrosis from obstruction, or tumors requiring further investigation. For the patient with abdominal pain, an ultrasound can often provide an immediate diagnosis, guiding treatment without the need for more invasive or radiation-intensive studies.
4. Vascular and Cardiac Evaluation
-
Primary Use: With Doppler ultrasound capabilities, it evaluates blood flow velocity and direction, used for diagnosing deep vein thrombosis, arterial stenosis, varicose veins, and for basic cardiac assessment.
-
How it helps: For the vascular surgeon and cardiologist, Doppler ultrasound makes blood flow visible—revealing clots in deep veins, blockages in arteries, and the direction and velocity of flow through vessels. For the patient with leg swelling, the test can rule out life-threatening DVT; for the patient with peripheral artery disease, it documents the location and severity of blockages.
5. Musculoskeletal Imaging
-
Primary Use: High-resolution linear probes allow detailed imaging of muscles, tendons, ligaments, and joints for diagnosing tears, sprains, inflammation, and guiding interventions like injections or aspirations.
-
How it helps: For the orthopedic surgeon, sports medicine physician, and rheumatologist, musculoskeletal ultrasound provides dynamic assessment of soft tissues—showing tendon tears with movement, revealing inflammation in real time, and guiding precise placement of therapeutic injections. For the athlete with a suspected tendon tear or the patient with chronic joint pain, ultrasound provides answers and guides treatment, often without the need for MRI.
SECONDARY & SUPPORTIVE USES
1. Point-of-Care Ultrasound: Its portability and ease of use make it ideal for rapid bedside assessment in emergency medicine, critical care, and anesthesiology. For the trauma patient, the FAST exam can reveal internal bleeding in seconds; for the critically ill, bedside ultrasound guides fluid resuscitation and vascular access.
2. Small Parts Imaging: Evaluates superficial structures like the thyroid, breast, testicles, and superficial soft tissue lumps. For the patient with a thyroid nodule, breast lump, or scrotal mass, ultrasound provides detailed characterization without radiation exposure.
3. Procedural Guidance: Provides real-time visualization for accurate needle placement during biopsies, fluid drainages, joint injections, and nerve blocks. For the patient undergoing a biopsy or injection, ultrasound guidance means the procedure is more accurate, safer, and less painful.
4. Pediatric Imaging: A preferred first-line imaging modality for children due to the lack of radiation, used for abdominal, hip, and cranial exams. For the child with suspected developmental dysplasia of the hip or abdominal pain, ultrasound provides answers while protecting developing tissues from radiation.
5. Urological Imaging: Assesses the kidneys, bladder, and scrotum, providing information about obstruction, residual urine volume, and testicular pathology. For the patient with urinary symptoms or scrotal pain, ultrasound provides rapid, non-invasive diagnosis.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Type: A diagnostic medical ultrasound system.
-
Common System Configuration:
-
Console: Cart-based system with an integrated computer, user interface (keyboard, trackball), and high-resolution LCD monitor.
-
Probes (Transducers): Supports multiple active array probes. A typical package includes:
-
Convex Array Probe (e.g., 3.5MHz): For general abdominal and obstetric imaging.
-
Linear Array Probe (e.g., 7.5MHz): For vascular, small parts, and musculoskeletal imaging.
-
Phased Array Probe (e.g., 2.5MHz): For cardiac and thoracic imaging.
-
Endocavitary Probe (optional): For gynecological and prostate imaging.
-
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Imaging Principle: Uses a transducer probe to emit high-frequency sound waves into the body. The waves reflect off tissues of different densities, and the echoes are received and processed to create a real-time image (sonogram).
-
Key Imaging Modes:
-
B-Mode (Brightness Mode): Standard 2D grayscale imaging.
-
M-Mode (Motion Mode): Shows motion of structures over time along a single line, used in cardiac imaging.
-
Doppler Modes: Color Doppler maps blood flow direction and velocity; Pulsed-Wave (PW) Doppler measures flow velocity at a specific point; Continuous-Wave (CW) Doppler measures high velocities along a line.
-
Harmonic Imaging: Improves image clarity by using tissue-generated harmonic frequencies, reducing artefacts.
-
-
Connectivity: DICOM 3.0 standard for sending images to a PACS (Picture Archiving and Communication System) and hospital network. USB ports for data export.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Portability: A cart-based system with lockable wheels, designed for mobility within a department (e.g., from radiology to patient bedside).
-
User Interface: Features an intuitive control panel, customizable user presets, and ergonomic design for operator comfort during prolonged scanning.
-
Monitor: A high-resolution, adjustable color display for optimal image viewing.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device.
-
Safety Standard: Complies with international standards (IEC 60601) for electrical and thermal safety. Ultrasound is considered very safe with no known ionizing radiation risk when used diagnostically.
-
ALARA Principle (As Low As Reasonably Achievable): Applies to acoustic output. Operators should use the lowest power output and shortest scan time necessary to obtain diagnostic information, especially during obstetric scanning.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry, temperature-controlled environment. The cart should be parked securely with brakes engaged.
-
Cleaning & Disinfection:
-
Probes: Wipe down with a hospital-grade disinfectant wipe after each patient. Critical: Follow manufacturer guidelines for disinfecting endocavitary probes (high-level disinfection or sterilization required).
-
Console and Cart: Wipe surfaces regularly with a mild disinfectant. Avoid liquid ingress into controls or ports.
-
-
Probe Care: Handle probes carefully. Store in designated holders. Never immerse non-waterproof connector ends. Check routinely for cable wear or transducer face damage.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: A versatile, foundational imaging tool used across hospital radiology departments, OB/GYN clinics, vascular labs, emergency rooms, outpatient imaging centers, and sports medicine facilities.
-
Operator-Dependent: Image quality and diagnostic accuracy are highly dependent on the skill and training of the sonographer or physician operator.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Infection Control: Strict adherence to probe cleaning protocols between patients is mandatory to prevent cross-contamination.
-
Thermal and Mechanical Index Monitoring: The system displays Thermal Index (TI) and Mechanical Index (MI) values. Operators should be aware of these, particularly in obstetric scanning, to avoid potential bio-effects from excessive energy output.
-
Electrical Safety: Ensure the power cord and connections are intact. Do not use it in the presence of flammable anesthetics.
-
Ergonomics: Sonographers should practice proper posture and scanning technique to prevent repetitive strain injuries.
2. FIRST AID MEASURES
-
Electrical Shock: Immediately disconnect power. Do not touch the patient or equipment. Call for emergency medical help. Begin CPR if trained and safe to do so.
-
Probe Damage/Liquid Ingress: Turn off the system. Unplug the damaged probe. Tag it for service. Do not attempt to use it.
3. FIRE FIGHTING MEASURES
-
Flammability: The plastic housing, monitor, and internal electronics are combustible.
-
Extinguishing Media: For electrical fires, use a CO₂ or dry chemical extinguisher. Evacuate and alert the fire department.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties