Blood Collection Tubes
WhatsApp Order
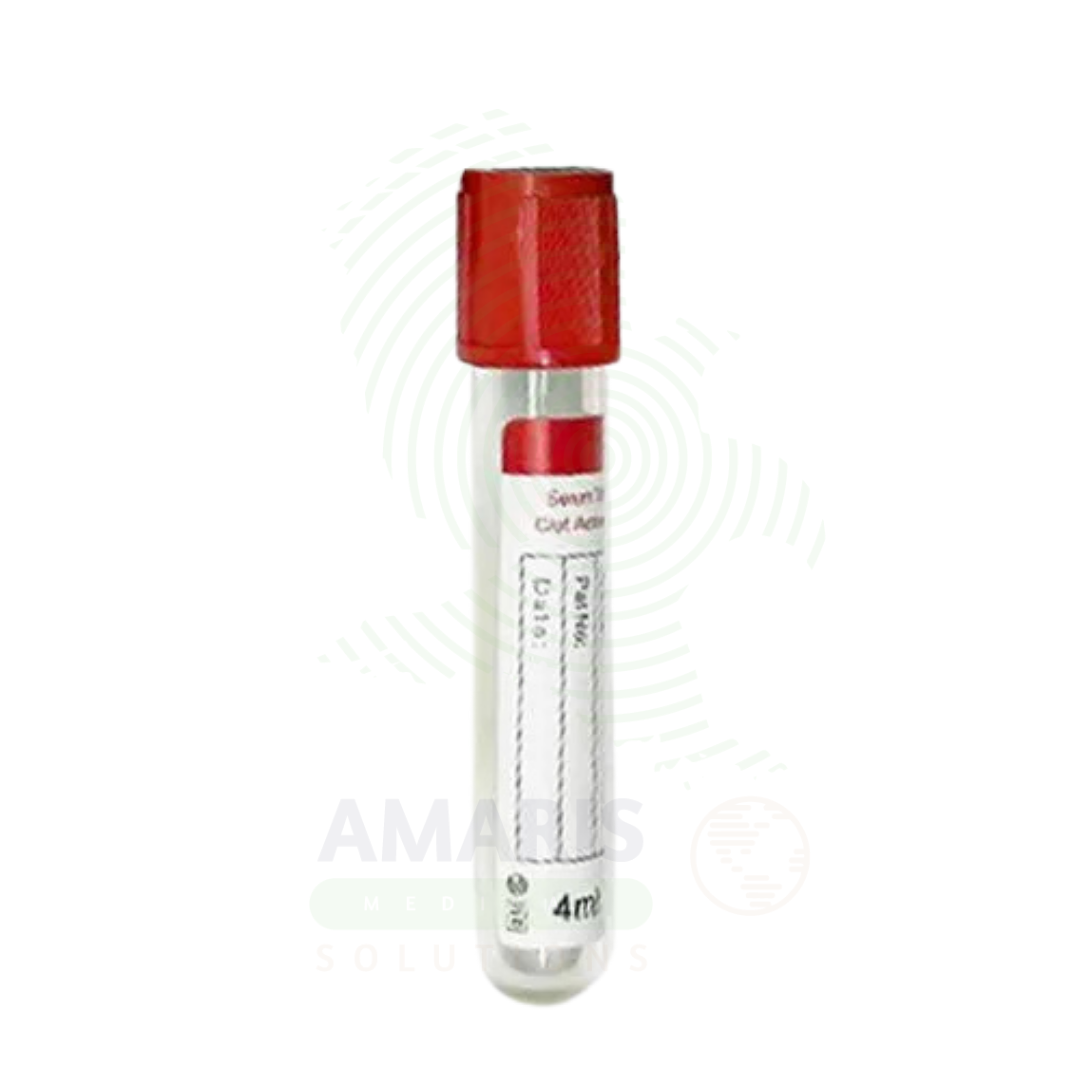
Blood Collection Tubes are sterile, evacuated tubes for collecting venous blood specimens for diagnostic testing. Color-coded by additive type, they ensure proper specimen preservation for chemistry, hematology, coagulation, and molecular testing. Essential for hospitals, clinics, and laboratories.
Description
Blood Collection Tubes
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Venous Blood Collection for Diagnostic Testing
-
Primary Use: Provides sterile, evacuated tubes for collecting venous blood specimens for laboratory analysis. The pre-measured vacuum draws a precise volume of blood directly from the vein, ensuring accurate blood-to-additive ratios essential for reliable test results.
-
How it helps: For the phlebotomist and laboratory technician, blood collection tubes standardize the specimen collection process—ensuring consistent volume, proper mixing with additives, and reliable results. For the patient, this means fewer repeat blood draws due to clotted or hemolyzed specimens and more accurate test results.
2. Additive-Specific Blood Preservation
-
Primary Use: Different tube types contain specific additives (anticoagulants, clot activators, preservatives, separation gels) that prepare blood specimens for particular diagnostic tests, ensuring optimal specimen integrity from collection to analysis.
-
How it helps: For the laboratory scientist, color-coded tubes with specific additives ensure that each specimen is collected in the optimal formulation for its intended test—preserving cellular elements, preventing clotting, or stabilizing analytes. For the patient, this means that a single blood draw can yield specimens for multiple tests, each collected in the tube that will preserve its unique characteristics for accurate analysis.
3. Standardization of Blood Collection
-
Primary Use: The evacuated tube system standardizes blood collection across healthcare settings, ensuring consistent specimen volume, correct blood-to-additive ratio, and uniform processing conditions, reducing pre-analytical errors.
-
How it helps: For the laboratory quality manager, standardized tubes reduce variability in specimen collection—improving test accuracy and reducing the need for recollection. For the patient, this means their test results are reliable and comparable across different facilities and over time.
4. Clot Activation for Serum Separation
-
Primary Use: Tubes containing clot activators (silica particles, thrombin) accelerate the clotting process, allowing rapid separation of serum for chemistry, immunology, and serology testing.
-
How it helps: For the laboratory technician, clot activator tubes enable faster processing of serum specimens—reducing turnaround time for critical results. For the patient, this means faster availability of test results for clinical decision-making.
5. Anticoagulation for Plasma and Whole Blood Testing
-
Primary Use: Tubes containing anticoagulants (EDTA, heparin, citrate) prevent clotting, preserving cellular components for hematology, coagulation, and molecular testing.
-
How it helps: For the hematology and coagulation laboratory, anticoagulated tubes ensure that specimens arrive in optimal condition for accurate cell counts, coagulation studies, and molecular assays. For the patient, this means accurate results for critical tests like complete blood counts, PT/INR, and blood cultures.
SECONDARY & SUPPORTIVE USES
1. Blood Culture Collection: Specialized tubes with culture media are used for detecting bacteremia and fungemia. For the microbiologist, blood culture bottles provide the growth medium needed to identify bloodstream infections; for the patient with suspected sepsis, this means rapid identification of the causative organism and targeted antibiotic therapy.
2. Trace Element Analysis: Tubes specially processed to minimize trace metal contamination are used for heavy metal testing and nutritional assessments. For the toxicologist, these tubes ensure accurate measurement of trace elements; for the patient undergoing environmental exposure assessment or nutritional evaluation, this means reliable results for guiding treatment.
3. Genetic and Molecular Testing: Tubes with preservatives for DNA and RNA stability are used for PCR, sequencing, and other molecular diagnostic tests. For the molecular biologist, these tubes protect nucleic acids from degradation; for the patient undergoing genetic testing or viral load monitoring, this means accurate results that guide diagnosis and treatment.
4. Therapeutic Drug Monitoring: Tubes with appropriate additives are used for measuring medication levels in patients receiving drugs with narrow therapeutic windows. For the pharmacist and clinician, accurate drug levels guide dosing adjustments; for the patient on medications like anticonvulsants, immunosuppressants, or cardiac drugs, this means optimal dosing that maximizes efficacy while minimizing toxicity.
5. Blood Bank and Transfusion Testing: Tubes are used for blood typing, antibody screening, and crossmatching. For the transfusion medicine specialist, these tubes provide the specimens needed for safe blood transfusion; for the patient receiving a blood transfusion, this means compatibility testing that prevents life-threatening transfusion reactions.
6. Research and Clinical Trials: Used for collecting specimens for research studies, biomarker discovery, and clinical trial testing. For the research scientist, standardized collection tubes ensure data integrity; for the patient participating in research, this contributes to medical knowledge and future treatments.
7. Pediatric Blood Collection: Smaller-volume tubes are designed specifically for pediatric patients to minimize blood loss. For the pediatric phlebotomist, these tubes allow necessary testing while respecting the child’s smaller blood volume; for the child and parents, this means fewer needle sticks and reduced risk of iatrogenic anemia.
8. Point-of-Care Testing Integration: Some tubes are designed for direct interfacing with point-of-care analyzers. For the clinician at the bedside, this enables rapid test results; for the patient, this means faster diagnosis and immediate treatment decisions.
9. Blood Donor Screening: Used to collect donor blood samples for mandatory infectious disease testing. For the blood bank, this ensures the safety of the blood supply; for the transfusion recipient, this means protection from transfusion-transmitted infections.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Product Type: Sterile, evacuated glass or plastic tubes for venous blood collection.
-
Designation: Blood Collection Tubes, Vacutainer Tubes, Venipuncture Tubes, Specimen Tubes.
-
Color Coding:
-
Lavender: EDTA (hematology, molecular)
-
Light Blue: Sodium Citrate (coagulation)
-
Red: No additive or clot activator (serum chemistry)
-
Gold/Tiger: Gel separator with clot activator (serum chemistry)
-
Green: Heparin (plasma chemistry)
-
Gray: Sodium fluoride/potassium oxalate (glucose, lactate)
-
Yellow: Acid citrate dextrose (blood bank, DNA)
-
-
Sizes: 2 mL, 3 mL, 4 mL, 5 mL, 6 mL, 7 mL, 8 mL, 10 mL, 15 mL.
-
Key Components:
-
Tube Body: Glass or PET plastic.
-
Additive: Anticoagulant, clot activator, or preservative.
-
Gel Separator: For serum or plasma separation.
-
Closure: Rubber stopper with color-coding.
-
Vacuum: Pre-measured for precise volume.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Vacuum: Pre-calibrated for specific fill volumes.
-
Additives: Manufactured to precise concentrations.
-
Sterility: Gamma irradiated or ethylene oxide sterilized.
-
Closure Integrity: Maintains vacuum until use.
-
Centrifugation: Gel tubes designed for specific centrifuge speeds.
-
Latex-Free: Stoppers available in latex-free formulations.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Clear for visualization of fill level and hemolysis.
-
Color Coding: Standardized for additive identification.
-
Labeling: Space for patient identification.
-
Packaging: Sterile, bulk or individually wrapped.
-
Disposal: Dispose in sharps or biohazard containers.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Sterility Assurance: Validated sterilization process.
-
Biocompatibility: Materials safe for blood contact.
-
CLSI Standards: Meets Clinical and Laboratory Standards Institute requirements.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store at room temperature; protect from heat and freezing.
-
Expiration: Check expiration date; do not use expired tubes.
-
Inspection: Do not use it if the vacuum is lost or the tube is damaged.
-
Disposal: Dispose in appropriate biohazard containers.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Collection and preservation of blood specimens for diagnostic testing.
-
Clinical Role: Essential equipment in hospitals, clinics, laboratories, and blood banks.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Order of Draw: Follow proper order of draw to prevent additive cross-contamination.
-
Fill Volume: Ensure tubes fill completely; underfilled tubes may have incorrect blood-to-additive ratio.
-
Mixing: Invert tubes gently to mix additives; do not shake vigorously.
-
Clotting: Allow serum tubes to clot fully before centrifugation.
-
Transport: Transport tubes upright and at appropriate temperature.
-
Inspection: Do not use tubes with lost vacuum or visible damage.
2. FIRST AID MEASURES
-
Needlestick: If needlestick occurs, follow institutional sharps injury protocol.
-
Broken Glass: If tube breaks, collect fragments carefully; dispose in a sharps container.
-
Additive Exposure: If additive contacts skin or eyes, rinse thoroughly; seek medical attention if irritation persists.
3. FIRE FIGHTING MEASURES
-
Flammability: Plastic and rubber components are combustible.
-
Extinguishing Media: Use water, foam, or CO₂ as appropriate for surrounding materials.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties