Magnetic Resonance Imaging
WhatsApp Order
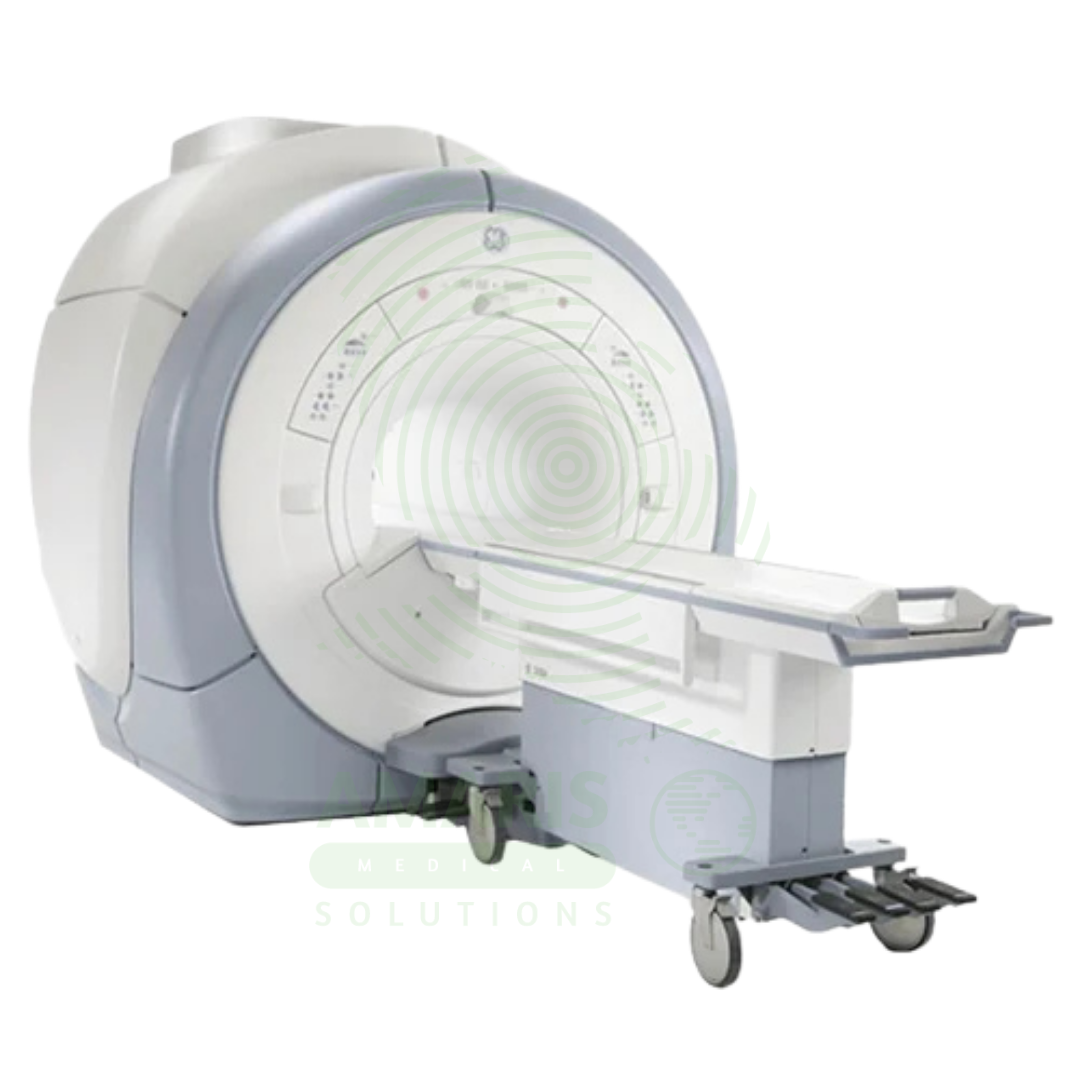
Magnetic Resonance Imaging (MRI) is a non-invasive diagnostic imaging modality that uses powerful magnetic fields and radiofrequency waves to produce detailed images of soft tissues, organs, and internal structures without ionizing radiation. It is the gold standard for imaging the brain, spinal cord, joints, muscles, and ligaments, and is essential for neurological, musculoskeletal, oncologic, and cardiovascular diagnosis. MRI provides exceptional soft tissue contrast, enabling precise anatomical characterization, tumor staging, and treatment planning. Strict safety protocols for ferromagnetic screening and contrast administration are essential for patient safety.
Description
Magnetic Resonance Imaging (MRI)
PRIMARY CLINICAL & DIAGNOSTIC USES
1. High-Contrast Soft Tissue Imaging
-
Primary Use: Produces exceptionally detailed images of soft tissues using powerful magnetic fields and radiofrequency waves without ionizing radiation. MRI is the gold standard for imaging the brain, spinal cord, nerves, muscles, ligaments, tendons, cartilage, and internal organs including the liver, prostate, uterus, and heart.
-
How it helps: For the radiologist and referring physician, MRI reveals the internal architecture of the human body with a clarity that no other imaging modality can match—distinguishing grey matter from white matter in the brain, revealing the internal structure of tumors, and showing the fine detail of ligaments, tendons, and cartilage. For the patient, an MRI means their condition can be diagnosed with confidence, often without exposure to radiation, and with sufficient detail to guide surgical planning, treatment decisions, and monitoring of disease progression.
2. Neurological and Neurosurgical Diagnosis
-
Primary Use: Critical for evaluating conditions including strokes (in subacute and chronic phases), multiple sclerosis, brain tumors, aneurysms, pituitary gland disorders, and degenerative diseases of the brain and spine such as Alzheimer’s disease, disc herniations, and spinal stenosis.
-
How it helps: For the neurologist and neurosurgeon, MRI provides an unprecedented window into the central nervous system—revealing the demyelinating plaques of multiple sclerosis, mapping the precise location and extent of brain tumors before surgery, and showing the compression of neural elements by herniated discs or spinal stenosis. For the patient with neurological symptoms, an MRI can provide definitive answers, distinguishing between treatable conditions and those requiring monitoring, and guiding decisions about surgery, medication, or watchful waiting.
3. Musculoskeletal System Evaluation
-
Primary Use: Provides unmatched detail for assessing joint injuries including knee meniscus and ligament tears, shoulder labral and rotator cuff tears, cartilage defects, bone marrow disorders, osteomyelitis, and soft tissue tumors.
-
How it helps: For the orthopedic surgeon and sports medicine specialist, MRI is indispensable for evaluating injuries that cannot be seen on X-ray—revealing torn menisci and cruciate ligaments in the knee, detecting labral tears in the shoulder, and identifying occult fractures and bone bruises. For the athlete with a suspected ligament tear or the patient with unexplained joint pain, an MRI provides the detailed anatomical information needed to determine whether surgery is necessary and to plan the procedure if it is.
4. Oncologic Imaging and Staging
-
Primary Use: Used for detecting, characterizing, and staging cancers, especially in the brain, spine, breast (with dedicated breast MRI), prostate (with multiparametric MRI), liver, and rectum. MRI is essential for surgical and radiation therapy planning, providing precise anatomical localization of tumors.
-
How it helps: For the oncologist, radiation therapist, and surgical oncologist, MRI provides the detailed anatomical roadmap essential for cancer care—defining the exact boundaries of tumors, revealing invasion into adjacent structures, detecting metastatic disease, and guiding biopsy and treatment planning. For the patient facing a cancer diagnosis, MRI provides the information needed to stage the disease accurately, plan treatment with precision, and monitor response to therapy over time.
5. Cardiovascular Imaging (Cardiac MRI)
-
Primary Use: Evaluates heart structure and function, detects myocardial damage from heart attacks, identifies cardiomyopathies, tumors of the heart, pericardial disease, and diseases of the large blood vessels including aortic dissection and aneurysms.
-
How it helps: For the cardiologist and cardiothoracic surgeon, cardiac MRI provides a comprehensive assessment of heart structure and function in a single examination—measuring ejection fraction, identifying areas of scar from prior heart attacks, detecting infiltrative diseases of the heart muscle, and evaluating complex congenital heart disease. For the patient with heart failure, suspected cardiomyopathy, or complex congenital heart disease, cardiac MRI provides the detailed information needed to guide treatment and predict outcomes.
SECONDARY & SUPPORTIVE USES
1. Functional MRI (fMRI): Maps brain activity by detecting blood flow changes during cognitive tasks, used in neurosurgery planning to identify eloquent cortex (speech, motor, sensory areas) before tumor resection, and in cognitive research.
2. Diffusion Weighted Imaging (DWI): Sensitive to the movement of water molecules, crucial for early detection of acute stroke within minutes of onset, and for characterizing tumors by assessing cellular density.
3. Magnetic Resonance Spectroscopy (MRS): Analyzes the biochemical composition of tissues, providing metabolic information that complements anatomical imaging for tumor characterization and metabolic disorder diagnosis.
4. MR Angiography (MRA): Visualizes blood vessels without contrast injection, used to detect aneurysms, arterial stenosis, dissections, and vascular malformations.
5. Diffusion Tensor Imaging (DTI): Maps white matter tracts in the brain, used for surgical planning and assessment of traumatic brain injury.
6. Interventional MRI: Provides real-time imaging guidance for biopsy needle placement and minimally invasive thermal ablation therapies.
7. Breast MRI: Used for screening high-risk patients, evaluating extent of breast cancer, and assessing response to neoadjuvant chemotherapy.
8. MR Cholangiopancreatography (MRCP): Non-invasive imaging of the biliary and pancreatic ducts for evaluation of stones, strictures, and tumors.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A medical imaging system that uses powerful magnetic fields and radiofrequency waves to generate detailed images of internal body structures.
-
Designation: MRI, Magnetic Resonance Imaging, MRI Scanner, MRI System.
-
Magnet Types:
-
Closed MRI: High-field cylindrical system providing superior image quality.
-
Open MRI: Lower-field system with open sides for claustrophobic or larger patients.
-
Wide-Bore MRI: Larger diameter bore for increased patient comfort.
-
Standing/Upright MRI: Allows imaging in weight-bearing positions.
-
-
Field Strength: Ranges from 0.2T to 3.0T for clinical use; 1.5T and 3.0T most common; higher field strengths (7T) used for research.
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Magnetic Field Strength: Measured in Tesla (T); higher field strength provides better signal-to-noise ratio and spatial resolution.
-
Magnet Type: Superconducting (most common), permanent, or resistive.
-
Bore Size: Standard bore 60-70 cm; wide bore 70-80 cm.
-
Image Acquisition: Multiple sequences (T1-weighted, T2-weighted, FLAIR, DWI, etc.) for different tissue characterization.
-
Contrast Agents: Gadolinium-based contrast used for enhancement of vascular structures, tumors, and inflammatory processes.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Construction: Large cylindrical magnet with patient table; housed in shielded room to contain magnetic field.
-
Patient Positioning: Patient lies supine on table that moves into magnet bore.
-
Noise Level: Significant acoustic noise during scanning; hearing protection required.
-
Scan Time: 20-60 minutes depending on protocol.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device regulated by FDA.
-
Magnetic Field Safety: Strict screening for ferromagnetic implants, devices, and foreign bodies.
-
Contraindications: Cardiac pacemakers, implantable defibrillators, certain aneurysm clips, cochlear implants, ferromagnetic foreign bodies.
-
Acoustic Safety: Hearing protection required due to high noise levels.
-
Claustrophobia: Some patients require sedation or open MRI systems.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Permanent installation in shielded MRI suite.
-
Quench Venting: Superconducting magnets require a venting system for emergency magnet quench.
-
Cryogen Management: Liquid helium required for superconducting magnet cooling.
-
Maintenance: Regular calibration and cryogen refills required.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Soft tissue imaging for neurological, musculoskeletal, oncologic, and cardiovascular diagnosis.
-
Clinical Role: Essential imaging modality in radiology, neurology, orthopedics, oncology, and cardiology.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Ferromagnetic Screening: Strict screening of all patients and personnel for ferromagnetic implants and objects.
-
Zone Management: Designated MRI safety zones (I-IV) with controlled access.
-
Quench Protocol: Emergency procedures for magnet quench with oxygen monitoring.
-
Contrast Safety: Screen for renal function before gadolinium administration to prevent nephrogenic systemic fibrosis.
-
Patient Monitoring: Monitor patients during scan; provide communication system for patient anxiety.
2. FIRST AID MEASURES
-
Quench: In event of magnet quench, evacuate area; monitor for oxygen displacement.
-
Patient Distress: If a patient experiences claustrophobia or panic, remove from the scanner immediately.
-
Contrast Reaction: Treat gadolinium contrast reactions per protocol; monitor for allergic response.
3. FIRE FIGHTING MEASURES
-
Flammability: Equipment is non-flammable; fire risk from electrical components.
-
Extinguishing Media: Use CO₂ or dry chemical extinguisher for electrical fires.
-
Magnetic Field Hazard: Use non-ferromagnetic extinguishers in MRI suite.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties