Mammography Machine
WhatsApp Order
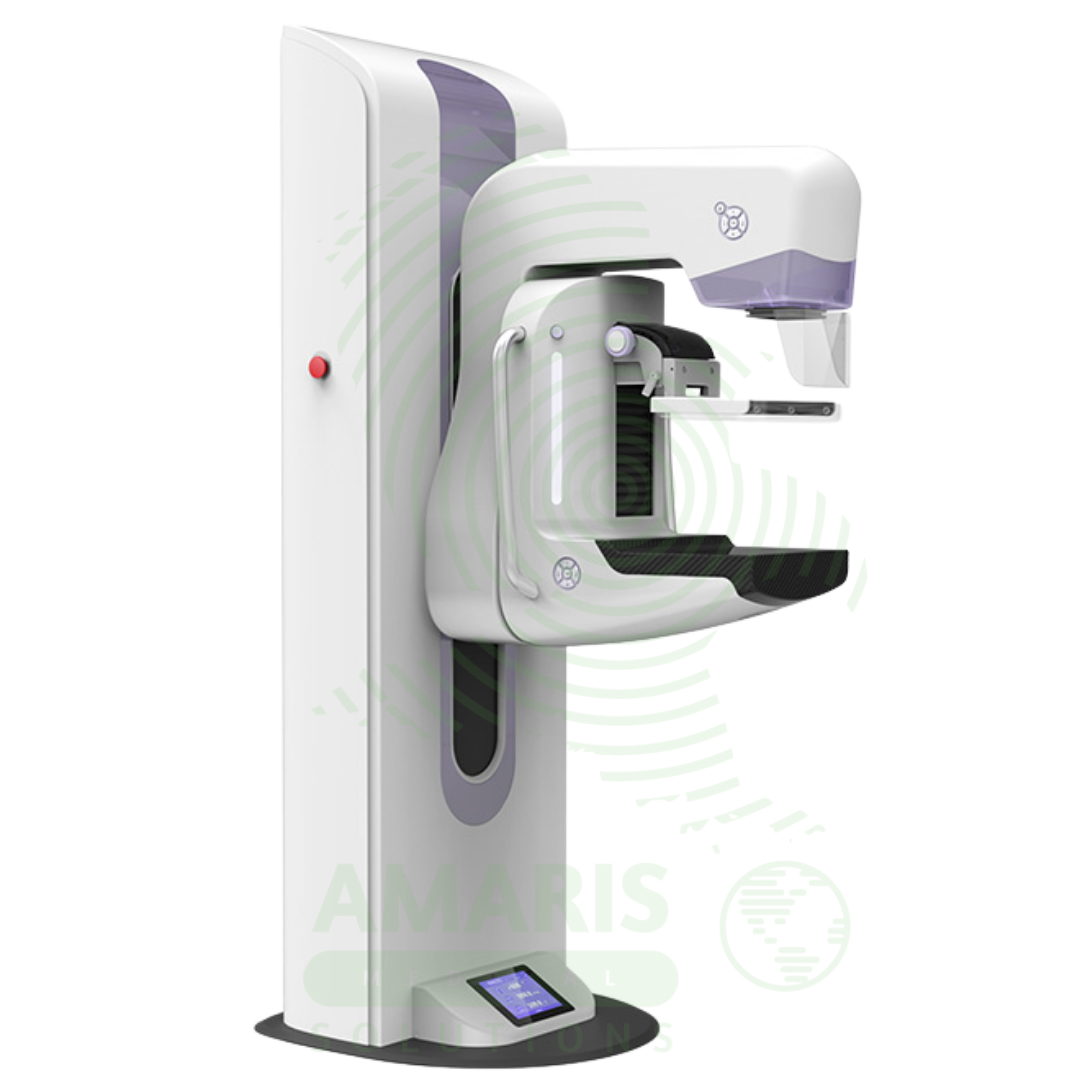
A Mammography Machine is a specialized, low-dose X-ray system designed exclusively for imaging the breast. It is the gold-standard tool for breast cancer screening and diagnostic evaluation, utilizing firm breast compression and high-resolution digital detectors to produce detailed images of breast tissue. Modern systems often incorporate Digital Breast Tomosynthesis (DBT or “3D mammography”) to reduce tissue overlap and improve cancer detection. Its operation is highly regulated, requiring certified technologists, qualified interpreting physicians, and a rigorous quality assurance program to ensure patient safety, optimal image quality, and accurate early detection of breast cancer, which is vital for reducing mortality.
Description
Mammography Machine
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Breast Cancer Screening
-
Primary Use: Provides routine screening of asymptomatic women to detect early, non-palpable breast cancer, significantly reducing mortality through early detection.
-
How it helps: For the radiologist and breast imaging specialist, screening mammography is the most powerful tool for finding breast cancer at its earliest, most treatable stage—detecting tumors years before they can be felt, identifying microcalcifications that signal early disease, and revealing subtle architectural distortions that warrant investigation. For the woman undergoing regular screening, a mammogram means peace of mind when results are normal and, when cancer is found, the best possible chance of cure with less aggressive treatment and better long-term outcomes.
2. Diagnostic Evaluation of Breast Symptoms
-
Primary Use: Investigates clinical signs such as a palpable lump, nipple discharge, skin changes, or persistent breast pain, using additional views and magnification to characterize abnormalities found on screening or during physical exams.
-
How it helps: For the breast surgeon and radiologist evaluating a patient with a concerning finding, diagnostic mammography provides the detailed characterization needed to determine the next steps—distinguishing benign from suspicious findings, mapping the extent of disease, and guiding biopsy decisions. For the patient who has found a lump or noticed a change in her breast, diagnostic imaging provides answers, whether the reassurance of a benign finding or the definitive diagnosis that allows treatment to begin.
3. Pre-operative Localization and Guidance
-
Primary Use: Guides needle localization procedures to mark non-palpable lesions for surgical biopsy or excision, and directs stereotactic core needle biopsies for precise tissue sampling without open surgery.
-
How it helps: For the breast surgeon and interventional radiologist, mammographic guidance transforms a blind surgical exploration into a precisely targeted procedure—placing localization wires exactly at the lesion site, guiding biopsy needles to the exact area of suspicion, and ensuring that the right tissue is sampled or removed. For the patient with a non-palpable abnormality, image-guided procedures mean a definitive diagnosis can be obtained with minimal discomfort and scarring, often avoiding the need for open surgical biopsy.
4. Monitoring and Follow-up
-
Primary Use: Provides surveillance for patients with a personal history of breast cancer or high-risk lesions to detect recurrence or new primary cancers.
-
How it helps: For the oncologist and breast surgeon managing breast cancer survivors, annual surveillance mammography is essential for detecting recurrences at an early, treatable stage—comparing current images with prior studies to identify subtle changes that might signal disease recurrence. For the patient who has already faced breast cancer, regular surveillance mammograms provide reassurance that she remains cancer-free and the earliest possible warning if a new disease appears.
5. Evaluation of Breast Implants
-
Primary Use: Specialized views are used to image breast tissue in patients with implants, assessing for rupture and detecting cancers that may be obscured by the implant.
-
How it helps: For the plastic surgeon and breast imager, dedicated implant views displace the implant backward while bringing breast tissue forward, allowing clear visualization of tissue that would otherwise be hidden. For the woman with breast implants, whether for reconstruction after cancer or cosmetic augmentation, specialized mammographic techniques ensure that her breast tissue is adequately screened despite the presence of implants.
SECONDARY & SUPPORTIVE USES
1. Assessment of High-Risk Patients: Used as part of a surveillance strategy for women with a strong family history or genetic predisposition to breast cancer, often starting at a younger age. For the woman with a BRCA mutation or other high-risk factors, earlier and more frequent screening provides the best chance for early detection.
2. Guiding Other Interventional Procedures: Can be used to guide other percutaneous breast procedures, such as cyst aspiration or abscess drainage. For the patient with a symptomatic breast cyst or infection, image guidance ensures accurate needle placement and successful treatment.
3. Research and Clinical Trials: Used to acquire standardized images for research studies on breast density, cancer risk, and the efficacy of new imaging technologies or treatments. For the advancement of breast cancer detection and treatment, mammography provides the standardized imaging essential for clinical research.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Type: A dedicated X-ray imaging system optimized for examining the breast.
-
Designation: Full-Field Digital Mammography (FFDM) System (modern standard) or Digital Breast Tomosynthesis (DBT) System (3D mammography, often combined with FFDM).
-
Common Variants:
-
2D Full-Field Digital Mammography (FFDM): Captures standard two-dimensional high-resolution images of the compressed breast.
-
Digital Breast Tomosynthesis (DBT or "3D Mammography"): Acquires a series of low-dose X-ray images from different angles, which are reconstructed into thin slices. This reduces tissue overlap, improving cancer detection and reducing false-positive recalls.
-
Contrast-Enhanced Mammography (CEM): An advanced technique where an iodinated contrast agent is injected, and dual-energy images are acquired to highlight areas of abnormal angiogenesis associated with tumors.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Imaging Principle: Uses low-dose X-rays. The breast is compressed between a paddle and a dedicated digital detector to spread tissue, reduce thickness (lowering dose), minimize motion blur, and improve image uniformity.
-
Key Components:
-
X-ray Tube with Molybdenum/Rhodium Anode: Produces an X-ray spectrum optimized for breast tissue contrast.
-
Compression Paddle: Applies firm, even compression. Automatic Exposure Control (AEC) sensors are integrated.
-
Digital Detector: A large-area flat-panel detector that converts X-rays directly into a digital image (Direct Radiography) or via a phosphor plate (Computed Radiography - now rare).
-
-
Image Quality Metrics: Spatial Resolution (measured in line pairs/mm, must be very high to see microcalcifications), Contrast Resolution, and Signal-to-Noise Ratio (SNR).
-
Dose: Uses low-dose radiation. Systems are designed to deliver the lowest possible dose while maintaining diagnostic image quality (ALARA principle).
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Gantry Design: Features a C-arm that rotates to allow standard craniocaudal (CC) and mediolateral oblique (MLO) views, as well as additional angles for diagnostic work.
-
Workstation: Includes a high-resolution review monitor and specialized software for image processing, Computer-Aided Detection (CAD) analysis, and comparison with prior studies.
-
Ergonomics: Designed for patient comfort and efficient technologist workflow, with intuitive controls and adjustable height.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device (radiation-emitting), subject to stringent regulatory oversight (e.g., FDA MQSA in the USA).
-
Quality Assurance (QA): Requires a rigorous, daily, weekly, and annual QA program mandated by law (under MQSA) to ensure consistent image quality, accurate dosage, and mechanical safety. This includes phantom imaging and testing of compression force.
-
Radiation Safety: Must comply with dose regulations. Technologists must be certified, and interpreting physicians must meet specific qualification requirements.
-
Compression Safety: Includes mechanisms to limit maximum force and allow the patient to self-release compression in an emergency.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: N/A – It is a fixed, installed piece of capital equipment.
-
Cleaning & Disinfection: The compression paddle, breast support table, and patient contact surfaces must be cleaned and disinfected after each patient using approved agents to prevent cross-contamination.
-
Preventive Maintenance: Requires scheduled service by specialized engineers to calibrate the X-ray tube, detector, and compression system, ensuring optimal performance and safety.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: The cornerstone of breast imaging, deployed in dedicated breast imaging centers, hospital radiology departments, and mobile screening vans.
-
Interpretation: Images are interpreted by radiologists with specialized training in breast imaging, often using comparison with prior mammograms and in conjunction with ultrasound or MRI.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Pregnancy Screening (CRITICAL): Always screen for possible pregnancy. Mammography is generally contraindicated during pregnancy due to fetal radiation exposure unless there is a strong clinical indication.
-
Patient Identification and Laterality: Meticulous protocol is required to ensure correct patient identification and accurate marking of right/left breast and view on every image. Errors can have catastrophic consequences.
-
Compression Technique: Proper compression is essential for image quality and dose reduction but must be applied with care and communication to minimize patient discomfort and anxiety.
-
Radiation Dose Monitoring: Ensure the AEC is functioning correctly and that the system is not operating outside its calibrated dose range.
-
Informed Consent: For screening, ensure patients understand the benefits, risks (including false positives and radiation exposure), and limitations of the exam.
2. FIRST AID MEASURES
-
Patient Injury from Compression (e.g., Pinch): Release compression immediately using the emergency release. Assess for injury and provide first aid. Document the incident.
-
Patient Faint or Fall: Lower the machine, support the patient, and call for clinical assistance.
-
Equipment Malfunction Causing Excessive Dose: This is a reportable event. Immediately take the machine out of service. Notify the Radiation Safety Officer (RSO) and service engineer.
3. FIRE FIGHTING MEASURES
-
Electrical Fire Hazard: Contains high-voltage components and electronics.
-
Extinguishing Media: Use CO₂ or dry chemical extinguishers. Evacuate and alert the fire department.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties