Breath Resuscitation Bag
WhatsApp Order
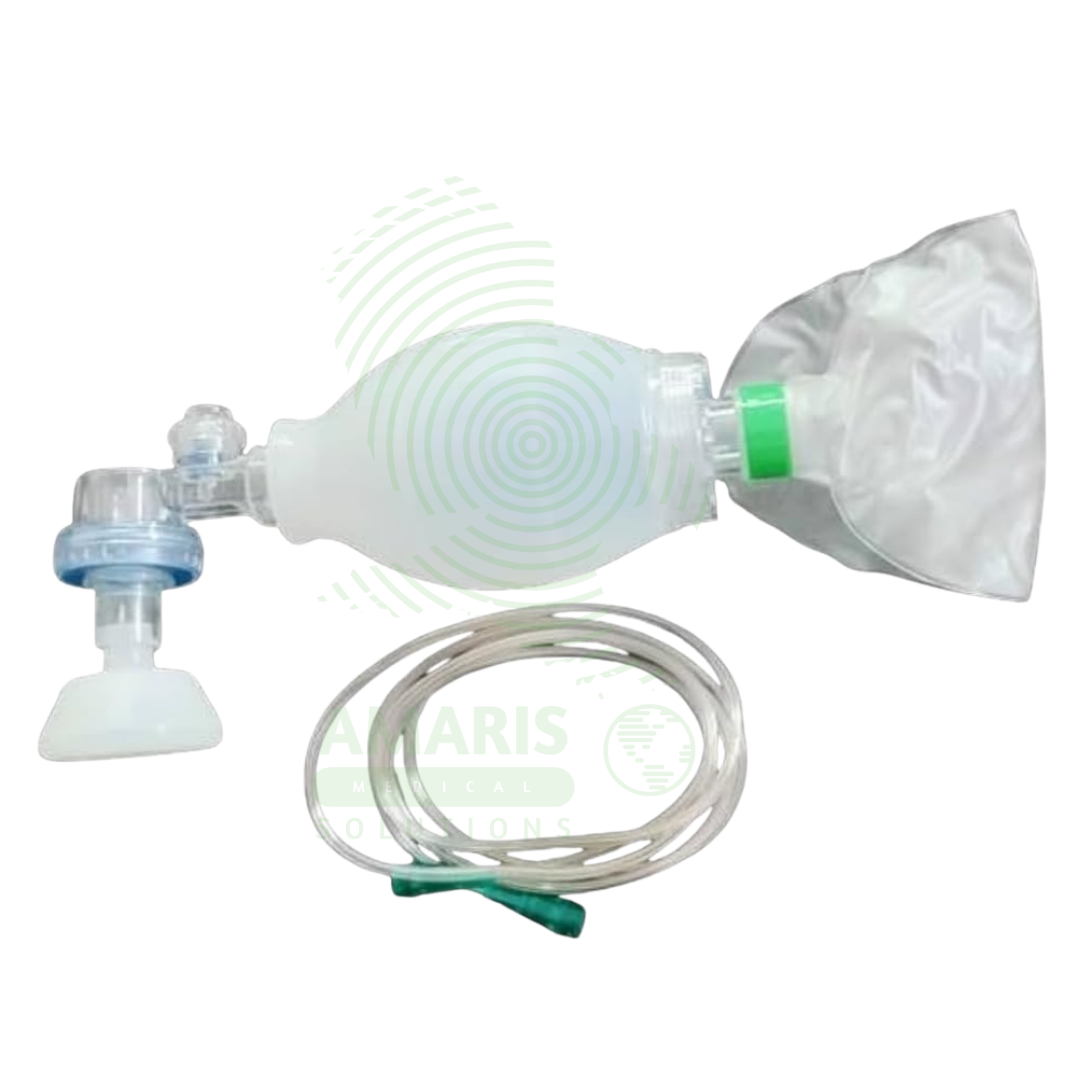
A Breath Resuscitation Bag (manual resuscitator, bag-valve-mask) is a Class II medical device used to deliver positive-pressure ventilation to patients in respiratory arrest, cardiac arrest, or respiratory failure. Available in adult (1,500-2,000 mL), pediatric (450-750 mL), and infant/neonatal (200-350 mL) sizes with self-inflating silicone or PVC bags, one-way non-rebreathing valves, transparent cushioned masks, and oxygen reservoirs for high FiO2 delivery (90-100% with reservoir). Oxygen inlet allows connection to flow meter (10-15 L/min recommended). Pediatric/neonatal models include pressure-limiting valves (35-45 cmH2O) to prevent barotrauma. Essential for CPR (AHA guidelines: adult 10-12 breaths/min, child 12-20, infant 20-30), preoxygenation before intubation, transport ventilation, and recovery from anesthesia. Critical safety considerations include avoiding excessive ventilation pressure (prevents gastric insufflation), maintaining proper mask seal, monitoring chest rise, and having backup equipment readily available. Indispensable emergency airway equipment in hospitals, ambulances, crash carts, and emergency response kits worldwide.
Description
Breath Resuscitation Bag
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Emergency Ventilation During Cardiopulmonary Resuscitation (CPR)
-
Primary Use: Provides positive-pressure ventilation to patients in respiratory arrest or cardiac arrest during CPR, delivering oxygen-enriched air until advanced airway management can be established.
-
How it helps: For the rescuer or code team member, it is their hands-on tool to literally breathe for the patient, buying precious minutes while others perform chest compressions or prepare medications. For the patient in cardiac arrest, each squeeze of the bag represents a chance—a delivery of life-sustaining oxygen to the brain and heart, extending the window of opportunity for successful resuscitation.
2. Respiratory Failure and Apnea Management
-
Primary Use: Used to ventilate patients with acute respiratory failure, apnea, or inadequate spontaneous breathing due to conditions such as opioid overdose, stroke, head injury, or drug-induced respiratory depression.
-
How it helps: For the emergency physician or first responder, it provides immediate, controllable ventilation the moment a patient stops breathing adequately, without waiting for equipment setup. For the patient, particularly in cases like opioid overdose, it is the difference between life and death—maintaining oxygen flow to the brain until the overdose can be reversed or the underlying condition treated.
3. Neonatal and Pediatric Resuscitation
-
Primary Use: Specialized pediatric and neonatal resuscitation bags with pressure-limiting features are essential in delivery rooms, NICUs, and pediatric emergency settings for ventilating newborns and children.
-
How it helps: For the neonatologist or pediatric nurse, pediatric-specific bags with pressure relief valves prevent the devastating lung injury that can occur from delivering adult-sized breaths to tiny lungs. For the newborn taking their first breaths or the child in respiratory distress, it provides gentle, age-appropriate support that matches their small anatomy and fragile lungs.
4. Preoxygenation Before Intubation
-
Primary Use: Used to preoxygenate patients before rapid sequence intubation, maximizing oxygen reserves during the apneic period before endotracheal tube placement.
-
How it helps: For the anesthesiologist or intensivist, it builds a critical oxygen “bank” in the patient’s lungs and blood, buying extra safe time to place the breathing tube without the patient desaturating. For the patient undergoing emergency intubation, those extra minutes of oxygen reserve can mean the difference between a controlled procedure and a crisis event.
5. Transport Ventilation
-
Primary Use: Provides manual ventilation during intra-hospital and inter-hospital transport of intubated or non-intubated patients when mechanical ventilators are not available or practical.
-
How it helps: For the transport team moving a patient through tight hallways or into an ambulance, it offers reliable, portable ventilation that doesn’t rely on batteries or power sources. For the critically ill patient being moved between departments or facilities, it ensures continuous respiratory support during the most vulnerable moments of their hospital journey.
6. Recovery from Anesthesia
-
Primary Use: Used in post-anesthesia care units (PACU) to manually ventilate patients recovering from general anesthesia who have delayed emergence or residual neuromuscular blockade.
-
How it helps: For the PACU nurse or anesthesiologist, it provides immediate support for the patient who is slow to wake or too weak to breathe adequately after surgery. For the post-surgical patient, it acts as a safety net—ensuring they continue to receive oxygen while their body metabolizes anesthetic drugs and regains the strength to breathe independently.
7. Disaster and Mass Casualty Response
-
Primary Use: Essential equipment in emergency response kits, disaster supplies, and mass casualty incidents where multiple patients may require immediate ventilatory support.
-
How it helps: For the disaster responder or field medic, it is a lightweight, durable, oxygen-free (can use room air) tool that can be deployed rapidly when resources are stretched thin. For victims of disasters, earthquakes, or mass casualty events, it represents basic life support capability in environments where sophisticated equipment is unavailable or overwhelmed.
SECONDARY & SUPPORTIVE USES
1. Respiratory Therapy Treatments: For the respiratory therapist, it serves as a delivery system for aerosolized medications. For the patient with severe bronchospasm, it combines life-saving ventilation with medication delivery in a single intervention.
2. Lung Recruitment Maneuvers: For the critical care team, it enables manual lung recruitment to open collapsed alveoli. For the patient with atelectasis, this manual technique can improve oxygenation and prevent the complications of collapsed lung tissue.
3. Manual Hyperinflation Therapy: For the respiratory therapist in the ICU, it helps prevent or treat atelectasis in intubated patients. For the ventilated patient, these manual breaths can loosen secretions and reinflate areas of collapsed lung, reducing the risk of pneumonia.
4. Teaching and Training: For the CPR instructor and clinical educator, it is the fundamental tool for teaching ventilation technique. For the healthcare student, mastering the bag-valve-mask is a core skill—one they will carry into every code, every arrest, and every respiratory emergency they face in their career.
5. Emergency Medical Services (EMS): For the paramedic and EMT, it is standard equipment on every ambulance, trusted and familiar. For the patient in the back of that ambulance, it represents the most basic and essential form of life support—someone breathing for them until they can breathe on their own again.
6. Military and Tactical Medicine: For the combat medic in the field, it is compact, durable, and does not require oxygen tanks that may be in short supply. For the wounded soldier, it provides critical ventilatory support during evacuation, maintaining life from the point of injury through transport to surgical care.
7. Veterinary Emergency Medicine: For the veterinarian, it provides the same life-saving capability for animal patients. For the pet owner facing an emergency with their beloved companion, it offers hope and advanced care options in the veterinary clinic.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Product Type: Hand-held manual resuscitator device for delivering positive-pressure ventilation to patients who are not breathing or breathing inadequately.
-
Common Names: Breath Resuscitation Bag, Manual Resuscitator, Bag-Valve-Mask (BVM), Ambu Bag (brand name), Resuscitation Bag, Manual Ventilation Device.
-
Components:
-
Self-Inflating Bag: Flexible silicone or PVC bag that self-inflates after compression; available in adult, pediatric, and neonatal sizes.
-
Patient Valve (Non-Rebreathing Valve): One-way valve directing gas flow to patient and preventing exhaled gases from re-entering the bag.
-
Mask: Transparent, cushioned mask for sealing over patient's nose and mouth (detachable; various sizes).
-
Oxygen Reservoir: Reservoir bag or tubing to collect oxygen for delivery of high FiO2 (up to 90-100% with reservoir).
-
Oxygen Inlet: Standard 22 mm fitting for connecting oxygen tubing from flow meter.
-
Pressure Limiting Valve: Some pediatric/neonatal models include pressure relief valves to prevent overinflation (typically 35-45 cmH2O).
-
Manometer Port: Some models have a port for connecting pressure manimeters to monitor ventilation pressures.
-
-
Sizes:
-
Adult: 1,500-2,000 mL bag volume
-
Pediatric: 450-750 mL bag volume
-
Infant/Neonatal: 200-350 mL bag volume
-
-
Materials: Medical-grade silicone (latex-free, durable, reusable) or PVC (disposable, economical).
-
Configuration: Disposable (single-patient use) or reusable (sterilizable between patients).
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Tidal Volume Delivery: Depends on bag size and operator technique; adult bag typically delivers 500-800 mL per compression.
-
Oxygen Delivery Capability:
-
Without Reservoir: 40-60% FiO2 (with oxygen flow 10-15 L/min).
-
With Reservoir: Up to 90-100% FiO2 (with adequate oxygen flow).
-
-
Valve Performance: Low resistance (≤2-3 cmH2O) for spontaneous breathing patients; minimal dead space.
-
Self-Inflating Feature: Bag automatically refills after compression; does not require gas source to operate (essential for backup).
-
Temperature Range: Functional from -18°C to +50°C (0°F to 122°F) for emergency use in various environments.
-
Pressure Relief (Pediatric/Neonatal): Pop-off valve activates at 35-45 cmH2O to prevent barotrauma.
-
Manometer Port: Allows real-time pressure monitoring during ventilation.
-
Oxygen Reservoir Efficiency: Collapsible reservoir bag fills during bag refill, conserving oxygen.
-
Mask Seal: Transparent masks allow visualization of vomitus, secretions, or cyanosis; cushioned rim for better seal.
-
Connection Ports: Standard 22 mm/15 mm ISO connectors for endotracheal tubes, tracheostomy tubes, and other airway devices.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Adult Bag Dimensions: 25-30 cm × 15-20 cm × 10-15 cm (approximate).
-
Weight: 300-800 grams depending on size and materials.
-
Bag Material: Silicone (reusable, autoclavable) or PVC (disposable, single-use).
-
Valve Material: Polycarbonate, polysulfone, or other medical-grade plastics.
-
Mask Material: Transparent PVC or silicone with soft cushion.
-
Oxygen Reservoir: Collapsible silicone or PVC bag (1-3 L capacity) or corrugated tubing.
-
Color Coding: Some manufacturers color-code by size: Adult (blue/green), Pediatric (orange), Infant/Neonatal (red/purple).
-
Storage: Compact; can be stored in emergency kits, crash carts, and ambulances.
-
Accessories: Carrying case, wall bracket, spare valves, PEEP valve attachments.
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Class II medical device requiring FDA 510(k) clearance; CE marked.
-
Clinical Standards: Complies with ISO 10651-4 (manual resuscitators) and ASTM F920 (performance requirements).
-
Latex-Free: All patient-contact components must be latex-free.
-
Valve Function: One-way valve must prevent rebreathing of exhaled gases.
-
Pressure Relief (Pediatric): Prevents excessive airway pressure (barotrauma) in vulnerable patients.
-
Self-Inflating: Bag must self-inflate within 1-2 seconds after compression at all temperatures.
-
Oxygen Inlet: Standard fitting; check valve prevents gas loss during bag refill.
-
Mask Transparency: Allows visualization of patient's mouth and nose for vomitus or secretions.
-
Dead Space: Minimal to prevent CO2 rebreathing.
-
Cleaning/Disinfection: Reusable models withstand repeated sterilization (autoclave, ETO, or chemical disinfection).
-
Quality Management: Manufactured under ISO 13485 certified processes.
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store in a clean, dry environment; protect from dust, extreme temperatures, and direct sunlight.
-
Preparation: Assemble bag, valve, mask, and oxygen reservoir before use; ensure all connections are secure.
-
Check Valve Function: Before use, test valve by compressing bag with mask covered; valve should direct flow properly.
-
Oxygen Connection: Connect oxygen tubing from flow meter (10-15 L/min for high FiO2) to oxygen inlet.
-
Mask Selection: Choose appropriate mask size for patients (neonatal, pediatric, adult).
-
Cleaning (Reusable): Disassemble; clean with mild detergent; rinse thoroughly; sterilize per manufacturer instructions.
-
Disposable Units: Single-use only; discard after use; do not resterilize or reuse.
-
Inspection: Before each use, check bag for cracks, valve for proper function, mask for seal integrity.
-
Expiration: Check expiration date on disposable units; do not use expired devices.
-
Emergency Preparedness: Keep readily accessible in crash carts, emergency kits, and ambulances.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: Emergency manual ventilation for patients in respiratory or cardiac arrest.
-
Resuscitation Techniques:
-
Bag-Valve-Mask (BVM) Ventilation: Mask sealed over nose and mouth; bag compressed to deliver breath; used for non-intubated patients.
-
Bag-to-Endotracheal Tube: Bag connected directly to ETT for ventilating intubated patients.
-
Bag-to-Tracheostomy Tube: Bag connected to tracheostomy tube for ventilating patients with tracheostomy.
-
-
Ventilation Parameters (AHA Guidelines):
-
Adult: 1 breath every 5-6 seconds (10-12 breaths/min); tidal volume sufficient for visible chest rise (approximately 500-600 mL).
-
Child (1 year to puberty): 1 breath every 3-5 seconds (12-20 breaths/min).
-
Infant (under 1 year): 1 breath every 2-3 seconds (20-30 breaths/min).
-
Neonate: 40-60 breaths/min (NRP guidelines).
-
-
Two-Person Technique: One person holds a mask with two hands to ensure seal; second person compresses a bag.
-
Oxygen Delivery:
-
Without Reservoir: Connect oxygen at 10-15 L/min → FiO2 40-60%.
-
With Reservoir: Connect oxygen at 10-15 L/min → FiO2 90-100%.
-
-
PEEP Application: Attach PEEP valve to patient valve outlet to maintain positive end-expiratory pressure.
-
Monitoring: Observe chest rise, auscultate breath sounds, monitor SpO2, and use a manometer (if available) to guide ventilation.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Avoid Gastric Insufflation: Excessive ventilation pressure forces air into the stomach, risking regurgitation and aspiration. Use appropriate tidal volume (just enough for visible chest rise) and maintain proper airway positioning.
-
Monitor Chest Rise: Deliver only enough volume to see chest rise; overinflation causes barotrauma and gastric insufflation.
-
Cricoid Pressure (Sellick Maneuver): May be used in appropriate patients to reduce gastric insufflation (controversial, follow current guidelines).
-
Mask Seal: Maintain good mask seal; leaks reduce ventilation effectiveness and cause eye irritation from air leak.
-
Oxygen Safety: Keep oxygen away from open flames and sparks; oxygen supports combustion.
-
Latex Allergy: Ensure latex-free components for patients and healthcare workers with latex allergy.
-
Single-Use Devices: Do not reuse disposable resuscitation bags; cross-contamination risk.
-
Valve Malfunction: If valve sticks or fails, replace immediately; have backup device available.
-
Temperature Extremes: Store within recommended temperature range; extreme cold may stiffen bag, extreme heat may degrade materials.
-
Training: All healthcare providers should be trained and regularly practice BVM ventilation techniques.
2. FIRST AID MEASURES
-
Ventilation Ineffective: Reposition airway (head tilt-chin lift or jaw thrust); check mask seal; clear airway of obstructions; consider two-person technique.
-
Vomiting During Ventilation: Immediately turn patient to side; clear airway; suction if available; resume ventilation.
-
Equipment Failure: Have backup resuscitation bags immediately available; replace defective units.
-
Oxygen Supply Failure: Continue ventilation with room air (bag self-inflates without oxygen); arrange alternative oxygen source.
3. FIRE FIGHTING MEASURES
-
Flammability: Bag and mask materials are combustible; oxygen supports combustion.
-
Extinguishing Media: Use CO₂ or dry chemical (Class C) extinguisher for electrical fires; water for surrounding materials.
-
Oxygen Source: Shut off oxygen if fire is suspected.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties