Defibrillator Monitor
WhatsApp Order
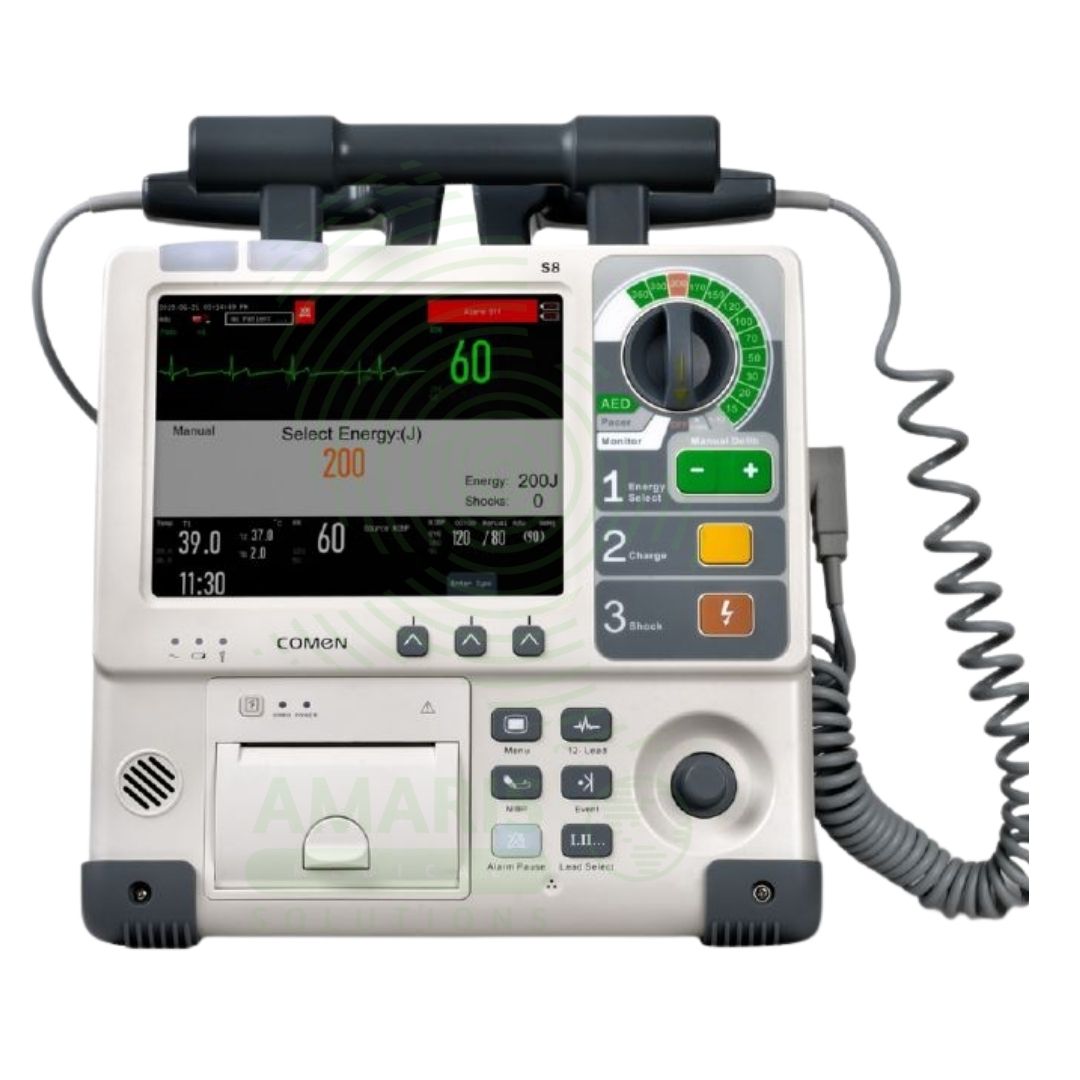
The Defibrillator Monitor is a critical, portable life-support device that combines continuous patient monitoring with immediate defibrillation and pacing capabilities. It is the frontline tool for managing cardiac arrest (through defibrillation) and unstable arrhythmias (through synchronized cardioversion or pacing) in emergency departments, during patient transport, and for hospital code teams. Essential for safe operation are rigorous daily self-tests, correct pad placement, and the strict protocol of clearing all personnel before delivering a shock. Its integrated monitoring of ECG, SpO2, and NIBP allows for comprehensive patient assessment at the point of greatest need.
Description
Defibrillator Monitor
PRIMARY CLINICAL & DIAGNOSTIC USES
1. Treatment of Life-Threatening Cardiac Arrhythmias
-
Primary Use: Delivers a therapeutic dose of electrical energy (defibrillation or synchronized cardioversion) to terminate ventricular fibrillation (VF), pulseless ventricular tachycardia (VT), and other unstable tachyarrhythmias, restoring an effective perfusing rhythm.
-
How it helps: For the code team, emergency physician, or paramedic, this device is the only intervention that can stop the chaotic, lethal quivering of a heart in arrest and give it a chance to beat normally again. For the patient in cardiac arrest, those joules delivered through the pads represent hope—the best chance to walk out of the hospital alive when their heart has forgotten how to beat.
2. Continuous Patient Monitoring
-
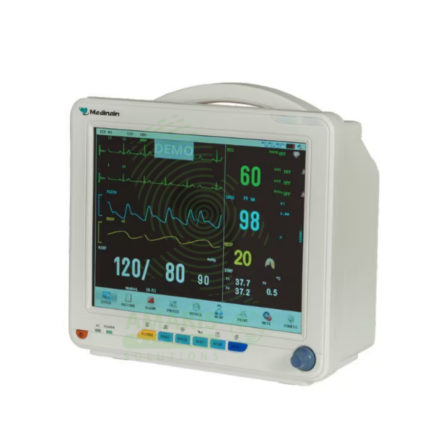
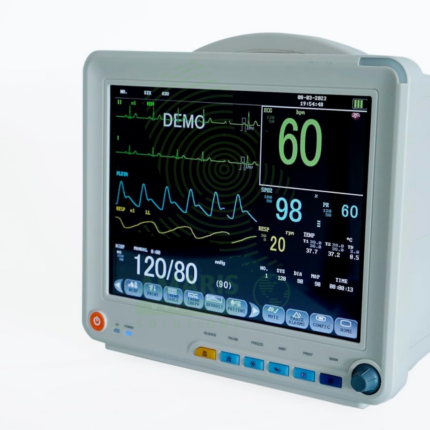
Primary Use: Provides real-time display and recording of essential vital signs, primarily electrocardiogram (ECG), but also non-invasive blood pressure (NIBP), pulse oximetry (SpO₂), and sometimes invasive pressures or temperature.
-
How it helps: For the critical care nurse and physician, it serves as the ever-watchful guardian at the bedside—tracking every heartbeat, every oxygen fluctuation, every blood pressure change while they attend to other tasks. For the unstable patient, this continuous surveillance means the moment a rhythm deteriorates or oxygen drops, help is immediately at the bedside, often before symptoms are even felt.
3. Pacing
-
Primary Use: Offers transcutaneous pacing (TCP) for patients with symptomatic bradycardia or asystole by delivering electrical impulses through external pads to stimulate cardiac contraction.
-
How it helps: For the clinician facing a patient with a heart rate so slow it cannot sustain life, the pacer function provides a temporary but life-saving bridge—externally commanding the heart to beat until a permanent pacemaker can be placed or the underlying cause reversed. For the patient in profound bradycardia, those electrical impulses mean blood continues to flow to the brain, consciousness is maintained, and vital organs remain perfused.
4. 12-Lead ECG Acquisition
-
Primary Use: Acquires, displays, and transmits a diagnostic-quality 12-lead electrocardiogram at the point of care, aiding in rapid diagnosis of conditions like acute myocardial infarction.
-
How it helps: For the emergency physician and cardiologist, a 12-lead ECG at the bedside or in the field provides the critical information needed to diagnose a heart attack in progress and activate the catheterization lab before the patient even arrives. For the patient with chest pain, this capability means faster diagnosis, faster treatment, and preserved heart muscle—directly translating to better outcomes and quality of life after a heart attack.
SECONDARY & SUPPORTIVE USES
1. Patient Transport: For the transport team moving a critically ill patient, the defibrillator monitor provides continuous surveillance and immediate intervention capability during the most vulnerable transitions. For the unstable patient being moved between units or facilities, this device ensures that monitoring and life support travel with them every step of the way.
2. Code Blue/Resuscitation Management: For the code team leader, the defibrillator monitor is the command center during a cardiac arrest—guiding rhythm interpretation, timing of shocks, and assessment of pulse with its integrated functions. For the patient in cardiac arrest, it provides the structured, protocol-driven care that gives the best chance of successful resuscitation.
3. Pre-Operative and Post-Operative Monitoring: For the anesthesiologist and PACU nurse, it monitors high-risk patients during the vulnerable periods before and after surgery when cardiac events are most likely to occur. For the surgical patient with known heart disease or risk factors, this vigilance provides an extra layer of safety during the stress of anesthesia and recovery.
KEY PRODUCT FEATURES
1. BASIC IDENTIFICATION ATTRIBUTES
-
Device Type: A portable, battery-powered, combined device integrating a cardiac monitor, defibrillator, and often a non-invasive pacemaker.
-
Core Functions: Monitor-Defibrillator-Pacer (often called an "MDP").
-
Core Components:
-
Main Console/Display: High-resolution color screen for waveform and parameter display.
-
Defibrillation Module: High-voltage capacitor and delivery system.
-
Battery Pack: Rechargeable, high-capacity lithium-ion battery for portability.
-
Patient Interface: Includes ECG cable and electrodes, defibrillation pads (adhesive, pre-connected), SpO2 sensor, NIBP cuff.
-
Controls: Dedicated knobs/buttons for energy selection, charge, and shock delivery, often with an integrated ECG recorder.
-
2. TECHNICAL & PERFORMANCE PROPERTIES
-
Defibrillation Energy: Maximum deliverable energy (e.g., 200J, 360J biphasic). Modern units use biphasic waveforms, which are more effective at lower energies than older monophasic waveforms.
-
Pacing Output: Current output for transcutaneous pacing (e.g., 0-200 mA).
-
Monitoring Parameters: Typically includes ECG (3/5/12-lead), SpO2, NIBP. May include etCO2 (capnography) and IBP modules.
-
Screen & Display: Size, resolution, and ability to display multiple parameters simultaneously.
-
Battery Life: Critical for portability, measured in hours of monitoring or number of shocks.
3. PHYSICAL & OPERATIONAL PROPERTIES
-
Portability: Designed as a rugged, portable unit on a wheeled cart or with carrying handles for rapid response.
-
Durability: Built to withstand the physical demands of emergency transport and use.
-
Data Management: Capabilities for data storage, review, and transmission to hospital networks or electronic medical records (EMR).
4. SAFETY & COMPLIANCE ATTRIBUTES
-
Regulatory Status: Classified as a Class II or III medical device (moderate to high risk) depending on features.
-
Electrical Safety: Must comply with IEC 60601-1 and the particular standard for defibrillators (IEC 60601-2-4).
-
Sync Mode for Cardioversion: Must have a synchronized mode that delivers the shock on the R-wave of the ECG to avoid inducing VF when cardioverting unstable atrial arrhythmias.
-
Impedance Compensation: Adjusts delivered energy based on patient transthoracic impedance to ensure the intended dose reaches the heart.
-
Safety Interlocks: Prevents accidental discharge and ensures shock is only delivered when intended (e.g., two-button press sequence, voice prompts).
5. STORAGE & HANDLING ATTRIBUTES
-
Storage: Store on its designated cart or charger in an accessible, ready-to-use location. The battery should be maintained on charge.
-
Daily/Pre-Use Check: Mandatory. Includes visual inspection, battery status check, and performing an operational self-test (which typically tests the defibrillation circuit using a built-in test load).
-
Cleaning & Disinfection: Wipe down the exterior, screen, and cables after each patient use with manufacturer-approved disinfectants. Avoid liquid ingress.
-
Accessory Inspection: Regularly check defibrillation pads and ECG electrodes for expiration dates and package integrity.
6. LABORATORY & CLINICAL APPLICATIONS
-
Primary Application: The essential life-support monitor for high-acuity and unpredictable environments: Emergency Departments, Intensive Care Units, Cardiac Care Units, and for hospital rapid response/code teams.
-
Clinical Role: Provides the critical link between monitoring for deterioration and having the immediate intervention tool (defibrillation/pacing) to treat it.
SAFETY HANDLING PRECAUTIONS
1. SAFETY PRECAUTIONS
-
Clear Before Shock (CRITICAL): Loudly announce "CLEAR!" and visually verify that no one is touching the patient or the bed before delivering a shock.
-
Pad Placement: For defibrillation, use antero-apical placement (sternum-apex). For pacing, use antero-posterior placement. Ensure pads make full skin contact; shave hair if necessary but do not delay.
-
Oxygen Safety: Do not deliver a shock in a oxygen-enriched atmosphere (e.g., directly under an oxygen mask or nasal cannula). Briefly move the source away or turn it off.
-
Pacing Discomfort: Transcutaneous pacing is painful for conscious patients. Sedation should be administered as soon as clinically feasible.
-
Water/Metal: Do not use the device if the patient or immediate environment is wet (risk of current arcing). Remove nitroglycerin patches from the chest wall (risk of arcing/burns).
2. FIRST AID MEASURES
-
Accidental Shock to Operator/Staff: If a rescuer is shocked, remove them from contact, assess for injury (cardiac monitoring if symptomatic), and provide standard first aid/burn care. The device must be inspected for fault.
-
Device Failure During Code: If the device fails to charge or deliver a shock, immediately switch to a backup unit or use manual CPR. Remove the faulty unit from service.
-
Skin Burns from Pads: If significant skin burns occur from pad placement, provide standard burn care after the acute event is stabilized.
3. FIRE FIGHTING MEASURES
-
Flammability: Plastic and electrical components are combustible. The high-voltage capacitor presents a significant energy source.
-
Extinguishing Media: In case of fire, disconnect from AC power if safe to do so. Use a CO2 or dry chemical (Class C) fire extinguisher. Do not use water.


 Dermatoscope and Magnifiers
Dermatoscope and Magnifiers Diagnostic Kits
Diagnostic Kits Vital Signs Monitors
Vital Signs Monitors Stethoscopes and Accessories
Stethoscopes and Accessories Otoscopes, Ophthalmoscopes, and Retinoscopes
Otoscopes, Ophthalmoscopes, and Retinoscopes Reflex Hammers and Neurological Tools
Reflex Hammers and Neurological Tools Scales and Measuring Devices
Scales and Measuring Devices Spirometers and Pulmonary Function Tests
Spirometers and Pulmonary Function Tests
 Electrosurgical Units and Accessories
Electrosurgical Units and Accessories Cutting Instruments
Cutting Instruments Grasping and Holding Instruments
Grasping and Holding Instruments Hemostatic Instruments
Hemostatic Instruments Specialized Surgical Sets
Specialized Surgical Sets Single-Use Procedure Trays and Packs
Single-Use Procedure Trays and Packs Surgical Drapes, Gowns, and Covers
Surgical Drapes, Gowns, and Covers Tissue Unifying Instruments
Tissue Unifying Instruments
 Radiation Protection
Radiation Protection X-Ray Machines and Accessories
X-Ray Machines and Accessories Ultrasound Systems and Probes
Ultrasound Systems and Probes MRI and CT Scanners
MRI and CT Scanners Radiology Consumables
Radiology Consumables Bone Densitometers
Bone Densitometers Fluoroscopy Equipment
Fluoroscopy Equipment Imaging Tables and Positioning Aids
Imaging Tables and Positioning Aids
 Microscopes and Accessories
Microscopes and Accessories Centrifuges and Separators
Centrifuges and Separators Analyzers
Analyzers Incubators and Ovens
Incubators and Ovens Pipettes, Dispensers, and Lab Glassware
Pipettes, Dispensers, and Lab Glassware Refrigerators, Freezers, and Storage Units
Refrigerators, Freezers, and Storage Units Lab Consumables
Lab Consumables Sterilizers and Autoclaves for Lab Use
Sterilizers and Autoclaves for Lab Use
 Multi-Parameter Monitors
Multi-Parameter Monitors Ventilators and Respiratory Support Devices
Ventilators and Respiratory Support Devices Defibrillators and AEDs
Defibrillators and AEDs Infusion Pumps and IV Systems
Infusion Pumps and IV Systems Patient Warmers and Cooling Devices
Patient Warmers and Cooling Devices Central Monitoring Stations
Central Monitoring Stations Accessories
Accessories
 Anesthesia Machines and Workstations
Anesthesia Machines and Workstations Oxygen Concentrators and Delivery Systems
Oxygen Concentrators and Delivery Systems Nebulizers and Inhalers
Nebulizers and Inhalers CPAP/BiPAP Machines
CPAP/BiPAP Machines Airway Management
Airway Management Anesthesia Masks, Circuits, and Bags
Anesthesia Masks, Circuits, and Bags Humidifiers and Heaters
Humidifiers and Heaters Respiratory Therapy Accessories
Respiratory Therapy Accessories
 First Aid Kits and Cabinets
First Aid Kits and Cabinets Emergency Resuscitation Equipment
Emergency Resuscitation Equipment Trauma Supplies
Trauma Supplies Emergency Carts and Crash Carts
Emergency Carts and Crash Carts Burn Care Products
Burn Care Products Bleeding Control
Bleeding Control Automated External Defibrillators (AEDs)
Automated External Defibrillators (AEDs) Transport and Evacuation
Transport and Evacuation
 Wheelchairs and Accessories
Wheelchairs and Accessories Walkers, Crutches, and Canes
Walkers, Crutches, and Canes Prosthetics and Orthotics
Prosthetics and Orthotics Physical Therapy Equipment
Physical Therapy Equipment Transfer Devices
Transfer Devices Bathroom Safety
Bathroom Safety Orthopedic Traction and Tables
Orthopedic Traction and Tables Hot/Cold Therapy Packs and Units
Hot/Cold Therapy Packs and Units
 Beds and Mattresses
Beds and Mattresses Chairs and Stools
Chairs and Stools Tables
Tables Cabinets and Storage
Cabinets and Storage Privacy Screens & Curtains
Privacy Screens & Curtains Stands and Racks
Stands and Racks Linens and Textiles
Linens and Textiles Lighting
Lighting
 Autoclaves and Sterilizers
Autoclaves and Sterilizers Ultrasonic Cleaners
Ultrasonic Cleaners Disinfectant Solutions and Wipes
Disinfectant Solutions and Wipes Sterilization Pouches, Wraps, and Indicators
Sterilization Pouches, Wraps, and Indicators Instrument Trays and Containers
Instrument Trays and Containers UV and Ozone Disinfection Devices
UV and Ozone Disinfection Devices Washer Disinfectors
Washer Disinfectors
 Wound Care
Wound Care Gloves
Gloves Masks and Respirators
Masks and Respirators Catheters and Tubing
Catheters and Tubing Swabs, Applicators, and Sponges
Swabs, Applicators, and Sponges Incontinence Products
Incontinence Products Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE)
 Dental Chairs and Units
Dental Chairs and Units Handpieces and Burs
Handpieces and Burs Instruments
Instruments Consumables
Consumables Sterilization for Dental Use
Sterilization for Dental Use Orthodontic Supplies
Orthodontic Supplies Endodontic Tools
Endodontic Tools
 Slit Lamps and Tonometers
Slit Lamps and Tonometers Lensometers and Phoropters
Lensometers and Phoropters Ophthalmic Surgical Instruments
Ophthalmic Surgical Instruments Eyewear Frames and Lenses
Eyewear Frames and Lenses Contact Lens Supplies
Contact Lens Supplies Vision Testing Charts and Devices
Vision Testing Charts and Devices Eye Care Consumables
Eye Care Consumables Laser Systems for Eye Care
Laser Systems for Eye Care
 ENT Exam Chairs and Tables
ENT Exam Chairs and Tables Endoscopes
Endoscopes Audiometers and Hearing Tests
Audiometers and Hearing Tests ENT Instruments
ENT Instruments Nasal and Throat Packs
Nasal and Throat Packs Hearing Aids and Accessories
Hearing Aids and Accessories Otology Supplies
Otology Supplies
 Fetal Dopplers and Monitors
Fetal Dopplers and Monitors Delivery Beds and Tables
Delivery Beds and Tables Gynecological Instruments
Gynecological Instruments Neonatal Incubators and Warmers
Neonatal Incubators and Warmers Breast Pumps and Accessories
Breast Pumps and Accessories Contraceptive Devices
Contraceptive Devices Maternity Supports and Pads
Maternity Supports and Pads Neonatal Consumables
Neonatal Consumables
 Cystoscopes and Urethroscopes
Cystoscopes and Urethroscopes Dialysis Machines and Supplies
Dialysis Machines and Supplies Urological Catheters and Bags
Urological Catheters and Bags Lithotripters
Lithotripters Prostate Treatment Devices
Prostate Treatment Devices Urinary Incontinence Products
Urinary Incontinence Products Kidney Stone Management Tools
Kidney Stone Management Tools Consumables & Disposables
Consumables & Disposables
 EEG and EMG Machines
EEG and EMG Machines Neurosurgical Instruments
Neurosurgical Instruments Nerve Stimulators
Nerve Stimulators Headrests and Positioning Aids
Headrests and Positioning Aids Lumbar Puncture Kits
Lumbar Puncture Kits Seizure Monitoring Devices
Seizure Monitoring Devices Consumables
Consumables Rehabilitation for Neurological Conditions
Rehabilitation for Neurological Conditions
 ECG Machines and Accessories
ECG Machines and Accessories Holter Monitors
Holter Monitors Stress Test Systems
Stress Test Systems Pacemakers and Defibrillator Accessories
Pacemakers and Defibrillator Accessories Vascular Access Devices
Vascular Access Devices Cardiac Catheters and Guidewires
Cardiac Catheters and Guidewires Blood Flow Meters
Blood Flow Meters Consumables
Consumables
 Orthopedic Instruments
Orthopedic Instruments Casts, Splints, and Padding
Casts, Splints, and Padding Joint Replacement Supplies
Joint Replacement Supplies Prosthetic Limbs and Components
Prosthetic Limbs and Components Bone Grafts and Substitutes
Bone Grafts and Substitutes Traction Devices
Traction Devices Orthopedic Braces and Supports
Orthopedic Braces and Supports Rehabilitation Aids for Orthopedics
Rehabilitation Aids for Orthopedics
 Home Oxygen Therapy
Home Oxygen Therapy Hospital Beds for Home Use
Hospital Beds for Home Use Mobility Aids
Mobility Aids Bathroom and Daily Living Aids
Bathroom and Daily Living Aids Wound Care for Home
Wound Care for Home Monitoring Devices
Monitoring Devices Enteral Feeding Pumps and Tubes
Enteral Feeding Pumps and Tubes
 Hand Sanitizers and Dispensers
Hand Sanitizers and Dispensers Face Shields and Goggles
Face Shields and Goggles Isolation Gowns and Suits
Isolation Gowns and Suits Biohazard Waste Containers
Biohazard Waste Containers Air Purifiers and HEPA Filters
Air Purifiers and HEPA Filters Surface Disinfectants
Surface Disinfectants Sharps Containers
Sharps Containers Protective Barriers
Protective Barriers
 Cardiovascular & Endurance Training
Cardiovascular & Endurance Training Strength Training & Weightlifting
Strength Training & Weightlifting Functional Training & Core Conditioning
Functional Training & Core Conditioning Physical Therapy & Rehabilitation
Physical Therapy & Rehabilitation Sports & Outdoor Recreation
Sports & Outdoor Recreation Gym Flooring & Facility Equipment
Gym Flooring & Facility Equipment Fitness Monitoring & Accessories
Fitness Monitoring & Accessories Kids & Novelties
Kids & Novelties